
Hematemesis, or vomiting blood, is often a sign of a serious underlying condition. While some cases of hematemesis are acute and can be treated effectively, others may become chronic, signaling long-term gastrointestinal (GI) issues. Chronic hematemesis can lead to severe health complications if left untreated.
In this blog, we’ll explore the risks and complications associated with chronic hematemesis, the conditions that can cause recurrent vomiting of blood, and the treatment strategies to manage the condition and prevent further complications.
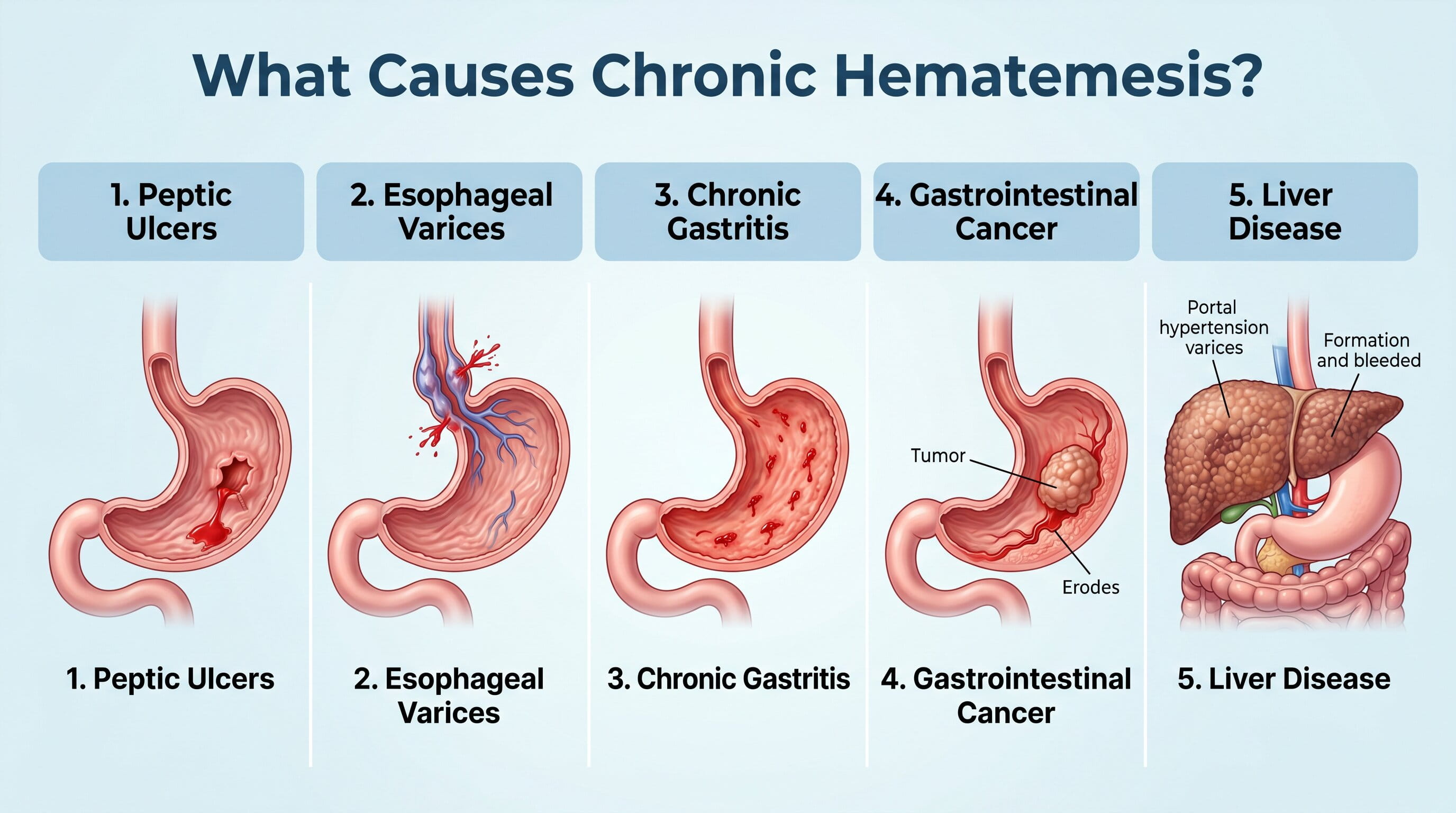
Chronic hematemesis is often a result of ongoing GI bleeding, which may be caused by conditions that damage the GI tract and interfere with normal function. The most common causes of chronic hematemesis include:
Peptic ulcers are open sores that develop in the stomach or duodenum, often caused by H. pylori infection or prolonged NSAID use. These ulcers can bleed intermittently, leading to chronic hematemesis. If left untreated, ulcers can worsen and cause significant blood loss.
Esophageal varices are swollen veins in the esophagus, often caused by liver cirrhosis. These veins can rupture and bleed over time, causing chronic vomiting of blood. The bleeding is typically slow and recurrent, requiring ongoing management.
Chronic gastritis, or long-term inflammation of the stomach lining, can be caused by factors such as alcohol use, H. pylori infection, or prolonged use of NSAIDs. Gastritis can lead to persistent bleeding, which results in vomiting blood.
In some cases, chronic hematemesis may be linked to gastrointestinal cancers, such as stomach cancer or esophageal cancer. These cancers can cause bleeding over an extended period, leading to recurrent vomiting of blood.
Chronic liver disease, especially cirrhosis, can lead to esophageal varices and portal hypertension, both of which increase the risk of recurrent bleeding and chronic hematemesis.
Chronic hematemesis can have serious health consequences if not properly managed. The risks and complications associated with chronic vomiting of blood include:
Repeated blood loss due to chronic hematemesis can lead to anemia, a condition in which the body does not have enough red blood cells to carry oxygen to the tissues. Symptoms of anemia include fatigue, weakness, and dizziness.
Severe or prolonged blood loss can lead to hypovolemic shock, a life-threatening condition where the body’s organs do not receive enough blood and oxygen. Shock requires immediate medical attention and can lead to organ failure if not treated.
Chronic vomiting, especially if accompanied by gastrointestinal bleeding, can interfere with the body’s ability to absorb nutrients. Over time, this can lead to malnutrition, which weakens the immune system and can slow the healing process.
In patients with chronic liver disease, the risk of liver failure increases with ongoing bleeding from esophageal varices. Liver failure can result in the inability to process toxins, produce essential proteins, or regulate blood flow, which can be fatal without a liver transplant.
Chronic hematemesis often requires repeated hospitalizations, which increases the risk of infections due to the need for invasive procedures or prolonged antibiotic use.
When chronic hematemesis is suspected, doctors will perform a series of tests to determine the cause of the bleeding and assess the severity of the condition. These may include:
An upper GI endoscopy (also known as an esophagogastroduodenoscopy) is the gold standard for diagnosing the source of chronic bleeding. During the procedure, a flexible tube with a camera is inserted through the mouth to examine the esophagus, stomach, and duodenum.
Blood tests, including a complete blood count (CBC) and liver function tests, are crucial for assessing the patient’s overall health and determining if anemia or liver damage is present.
In some cases, imaging studies like CT scans or ultrasound may be used to assess liver health, check for esophageal varices, or identify other potential sources of bleeding.
If an H. pylori infection is suspected as the cause of gastritis or peptic ulcers, a breath test, stool test, or blood test may be conducted to confirm the presence of the bacteria.
The treatment of chronic hematemesis depends on the underlying cause of the bleeding. Treatment strategies aim to control the bleeding, prevent recurrence, and address any associated conditions such as anemia or liver disease.
For patients with significant blood loss, blood transfusions may be required to restore red blood cell levels and prevent shock.
In severe cases, surgery may be necessary to remove the source of bleeding, such as a large ulcer, tumor, or section of the esophagus.
For patients with liver cirrhosis and esophageal varices, a liver transplant may be the only viable option to address both the liver disease and prevent recurrent bleeding.
Preventing chronic hematemesis involves managing the underlying causes and making lifestyle changes to reduce the risk of GI bleeding:
Excessive alcohol use is a major risk factor for liver disease and esophageal varices. Limiting alcohol intake or avoiding it completely can significantly reduce the risk of chronic hematemesis.

Smoking exacerbates the effects of ulcers and gastritis, making it more difficult for the digestive system to heal. Quitting smoking can improve overall digestive health.
If you have a history of ulcers or gastritis, avoiding long-term use of NSAIDs (like ibuprofen or aspirin) is important. Consider using alternatives like acetaminophen (Tylenol) for pain relief.
If you experience symptoms like frequent indigestion, stomach pain, or nausea, seek medical attention early to prevent ulcers or other conditions from progressing to more serious issues.
Chronic hematemesis is a serious condition that requires ongoing management to prevent complications such as anemia, liver failure, and shock. By addressing the underlying causes, such as peptic ulcers or liver disease, and following a treatment plan tailored to your needs, it is possible to manage chronic hematemesis and reduce the risk of severe health problems.
Yes, chronic hematemesis can be treated by addressing the underlying cause, whether it’s peptic ulcers, liver disease, or another condition. Treatments include medications, endoscopy, blood transfusions, and, in severe cases, surgery.
Long-term risks include anemia, shock, liver failure, and malnutrition. Untreated chronic bleeding can lead to severe complications and affect your overall health.
Chronic hematemesis is diagnosed through a combination of blood tests, endoscopy, and imaging studies to identify the source of bleeding and assess the severity of the condition.
Yes, lifestyle changes such as limiting alcohol consumption, quitting smoking, avoiding NSAIDs, and seeking early treatment for GI issues can significantly reduce the risk of chronic hematemesis.
No, while peptic ulcers are a common cause of chronic hematemesis, other conditions such as liver disease, esophageal varices, and gastrointestinal cancer can also lead to repeated vomiting of blood.