Hematemes is refers to the act of vomiting blood, a serious symptom of a problem in the upper gastrointestinal (GI) tract. It’s important to differentiate hematemesis from other conditions such as coughing up blood (hemoptysis) or vomiting due to a non-GI issue. Hematemesis often appears as bright red blood or as dark, coffee-ground-like material, indicating the blood’s exposure to stomach acid.
While vomiting blood is a concerning symptom, it’s not always an emergency. However, it could signal a wide range of GI issues, some of which require immediate medical attention. Identifying the cause of the bleeding is crucial for determining the right treatment.
Understanding the Causes of Hematemesis
Hematemesis can arise from various causes within the upper GI tract, including the esophagus, stomach, and duodenum. Some causes of hematemesis are mild and treatable, while others can be life-threatening. Below, we will explore the most common causes of hematemesis and how they are treated.
1. Peptic Ulcers
Peptic ulcers are sores that develop in the stomach lining or the first part of the small intestine (duodenum). These ulcers can bleed when they erode blood vessels. The most common cause of peptic ulcers is infection with Helicobacter pylori, a bacteria that disrupts the stomach lining, or prolonged use of nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or aspirin.
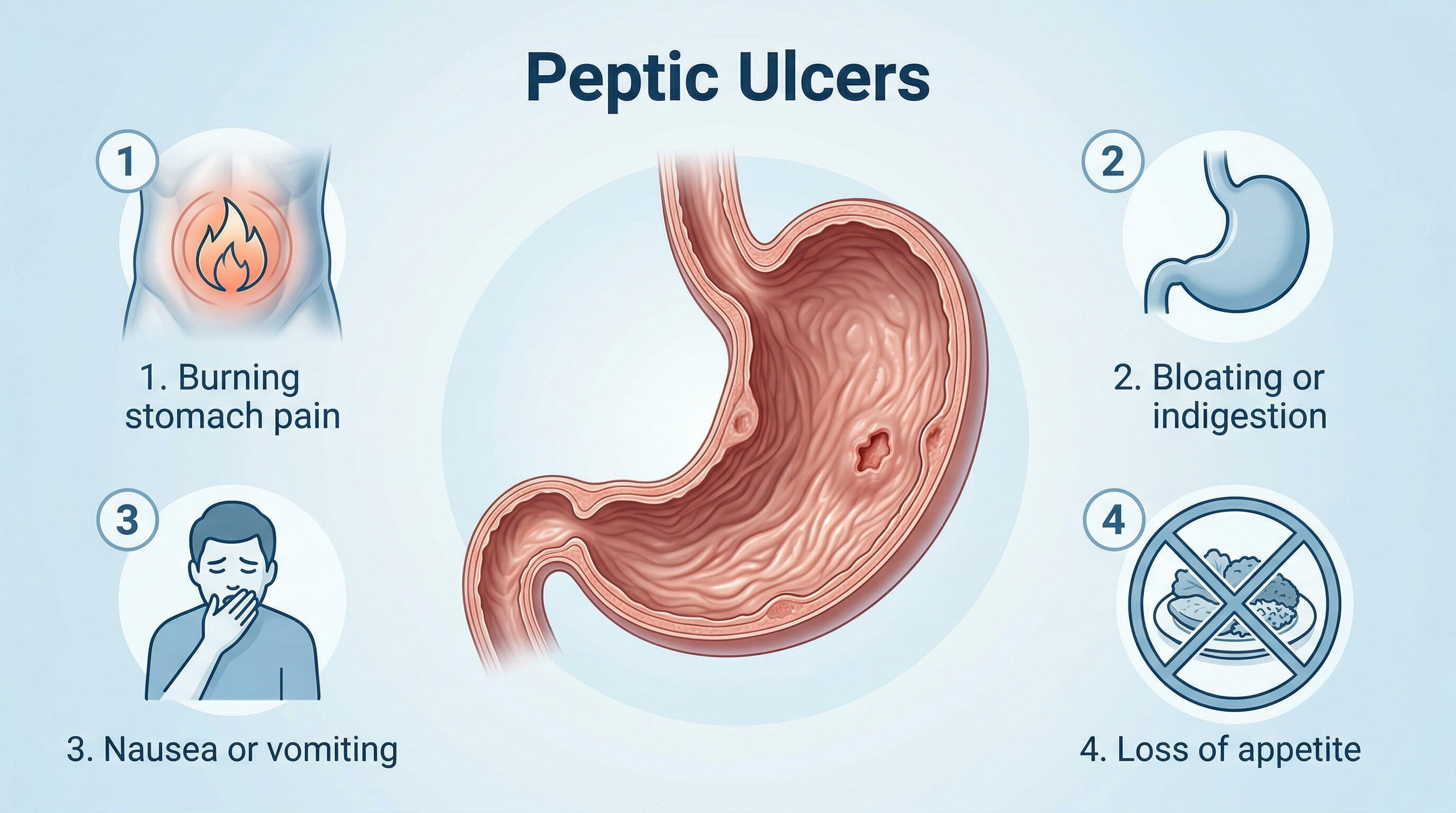
Symptoms of Peptic Ulcers:
- Burning stomach pain
- Bloating or indigestion
- Nausea or vomiting
- Loss of appetite
Diagnosis and Treatment:
Peptic ulcers are typically diagnosed through endoscopy or breath tests for H. pylori infection.
The treatment plan often involves:
- Proton pump inhibitors (PPIs) or H2 blockers to reduce stomach acid
- Antibiotics to treat H. pylori infection
- Discontinuing NSAIDs if they are the cause
- In severe cases, surgical intervention may be necessary.
2. Esophageal Varices
Esophageal varices are swollen veins in the lower esophagus that develop due to high blood pressure in the portal vein, often as a result of liver cirrhosis. These veins can rupture, leading to massive bleeding and vomiting of blood.
Symptoms of Esophageal Varices:
- Vomiting blood (sometimes profusely)
- Black or tarry stools (melena)
- Jaundice (yellowing of the skin or eyes)
- Swelling in the abdomen and legs
Diagnosis and Treatment:
Diagnosis typically involves an upper GI endoscopy, where doctors can visualize the varices and assess the extent of bleeding.
Treatment involves:
- Banding or sclerotherapy (to stop bleeding)
- Beta-blockers to reduce portal pressure
- Liver disease management and, in some cases, liver transplantation
3. Gastritis
Gastritis is inflammation of the stomach lining, which can result from infection, alcohol consumption, stress, or NSAID use. Severe cases of gastritis can lead to erosion of the stomach lining, causing bleeding and hematemesis.
Symptoms of Gastritis:
- Stomach pain or burning sensation
- Nausea or vomiting
- Indigestion
- Loss of appetite
Diagnosis and Treatment:
An endoscopy may be used to visualize the inflammation and rule out other conditions.
Treatment typically includes:
- PPIs or H2 blockers to reduce stomach acid
- Antibiotics if H. pylori infection is present
- Avoiding NSAIDs and alcohol
4. Mallory-Weiss Tear
A Mallory-Weiss tear is a tear in the mucous membrane where the esophagus meets the stomach. It typically occurs after forceful vomiting or retching. The tear can bleed, leading to hematemesis.
Symptoms of Mallory-Weiss Tear:
- Vomiting blood after a period of severe vomiting
- Abdominal pain or discomfort
Diagnosis and Treatment:
- Mallory-Weiss tears are diagnosed via endoscopy.
- Most cases heal on their own with rest and hydration.
- In severe cases, intervention such as cauterization or suture may be required.
5. Gastrointestinal Bleeding Disorders
Certain blood disorders, such as low platelet counts or clotting factor deficiencies, can increase the risk of bleeding in the GI tract. This may result in hematemesis.
Symptoms of Bleeding Disorders:
- Easy bruising
- Frequent nosebleeds
- Bleeding gums
- Hematemesis or melena
Diagnosis and Treatment:
- Blood tests can help diagnose clotting disorders.
- Treatment may include blood transfusions, clotting factor replacement, or other interventions to manage the bleeding.
6. Gastric Cancer
Though rare, stomach cancer (gastric cancer) can be a cause of hematemesis. Tumors in the stomach may erode into blood vessels, causing bleeding that presents as vomiting blood.
Symptoms of Gastric Cancer:
- Unexplained weight loss
- Nausea or vomiting
- Abdominal pain
- Feeling full after eating a small amount of food
Diagnosis and Treatment:
- Gastric cancer is diagnosed through endoscopy and biopsy.
- Treatment depends on the stage of the cancer and may include surgery, chemotherapy, and radiation therapy.
When to Seek Emergency Medical Care
Hematemesis should always be taken seriously. Even if the amount of blood is small, seeking immediate medical attention is crucial. Here are some signs that indicate hematemesis may be an emergency:
- Large amounts of blood: If the blood appears to be gushing or if vomiting blood is ongoing, immediate medical intervention is needed.
- Signs of shock: Symptoms like dizziness, confusion, and a rapid heartbeat can signal shock, which is a life-threatening condition.
- Severe abdominal pain: Intense, sharp abdominal pain accompanying vomiting blood may suggest a serious condition, such as an ulcer or gastrointestinal rupture.
- Persistent bleeding: If vomiting blood persists for more than a few minutes, seek help immediately.
- Underlying health conditions: People with chronic liver disease, known gastrointestinal issues, or a history of heavy alcohol use should seek immediate medical help if they experience hematemesis.
Diagnosis of Hematemesis
When hematemesis occurs, a thorough evaluation is necessary to determine the underlying cause. The diagnostic process may include the following:
1. Endoscopy (Upper GI)
An upper GI endoscopy is the most common procedure used to diagnose the source of bleeding. A flexible tube with a camera is inserted through the mouth to examine the esophagus, stomach, and duodenum. This allows doctors to identify ulcers, varices, tears, or tumors.
2. Blood Tests
Blood tests help assess the severity of blood loss, check for anemia, and evaluate liver function. They may also be used to screen for H. pylori infection or other underlying causes.
3. Imaging Studies
In some cases, imaging tests such as a CT scan may be needed to identify sources of bleeding that are not visible on endoscopy. This is particularly useful if esophageal varices or gastric cancer is suspected.
Treatment Options for Hematemesis
Treatment for hematemesis varies based on the underlying cause. The first step is to stabilize the patient, especially if there is significant blood loss. Once the patient is stable, the cause of the bleeding is addressed.
1. Intravenous Fluids and Blood Transfusions
For patients with significant blood loss, IV fluids are administered to stabilize the patient’s blood pressure and hydration. In severe cases, blood transfusions may be necessary to replenish lost blood.
2. Medications
Medications such as proton pump inhibitors (PPIs) or H2 blockers are commonly prescribed to reduce stomach acid and promote healing of ulcers or gastritis. In cases of H. pylori infection, antibiotics are used.
3. Endoscopic Treatments
Endoscopic treatments like banding or sclerotherapy are used to stop bleeding from esophageal varices or ulcers. Cauterization may also be performed to seal off the bleeding vessel.
4. Surgery
In cases where bleeding cannot be controlled with medications or endoscopy, surgery may be required. This is typically necessary for severe cases of peptic ulcers, gastric cancer, or ruptured esophageal varices.
Conclusion
Hematemesis is a serious medical condition that requires prompt attention. The causes range from common and treatable issues like ulcers and gastritis to more severe conditions like esophageal varices or gastric cancer. Understanding the causes and symptoms of hematemesis, as well as knowing when to seek medical care, can make a significant difference in the outcome of treatment. If you experience vomiting blood, it is important to seek immediate medical help to determine the cause and receive the appropriate treatment.