
Hematemesis (vomiting blood) is a serious and often frightening symptom that indicates bleeding in the upper gastrointestinal (GI) tract. If you or someone you know experiences vomiting blood, it’s important to understand what happens next, from diagnosis to treatment.
Hematemsis can occur due to various causes, including peptic ulcers, esophageal varices, and gastrointestinal cancers. While vomiting blood is a medical emergency, the right steps taken immediately after experiencing it can improve the chances of a positive outcome.
This step-by-step guide will walk you through what to expect during the medical process when experiencing hematemesis, from initial evaluation to treatment options and recovery.
If you experience vomiting blood, the first step is to assess the situation. Hematemesis can be recognized by:
It is important to seek immediate medical help if:
Once you seek medical attention, the healthcare team will immediately evaluate your condition and stabilize you. This initial evaluation focuses on assessing the severity of blood loss and preventing further complications.
The doctor will perform a physical exam to assess:
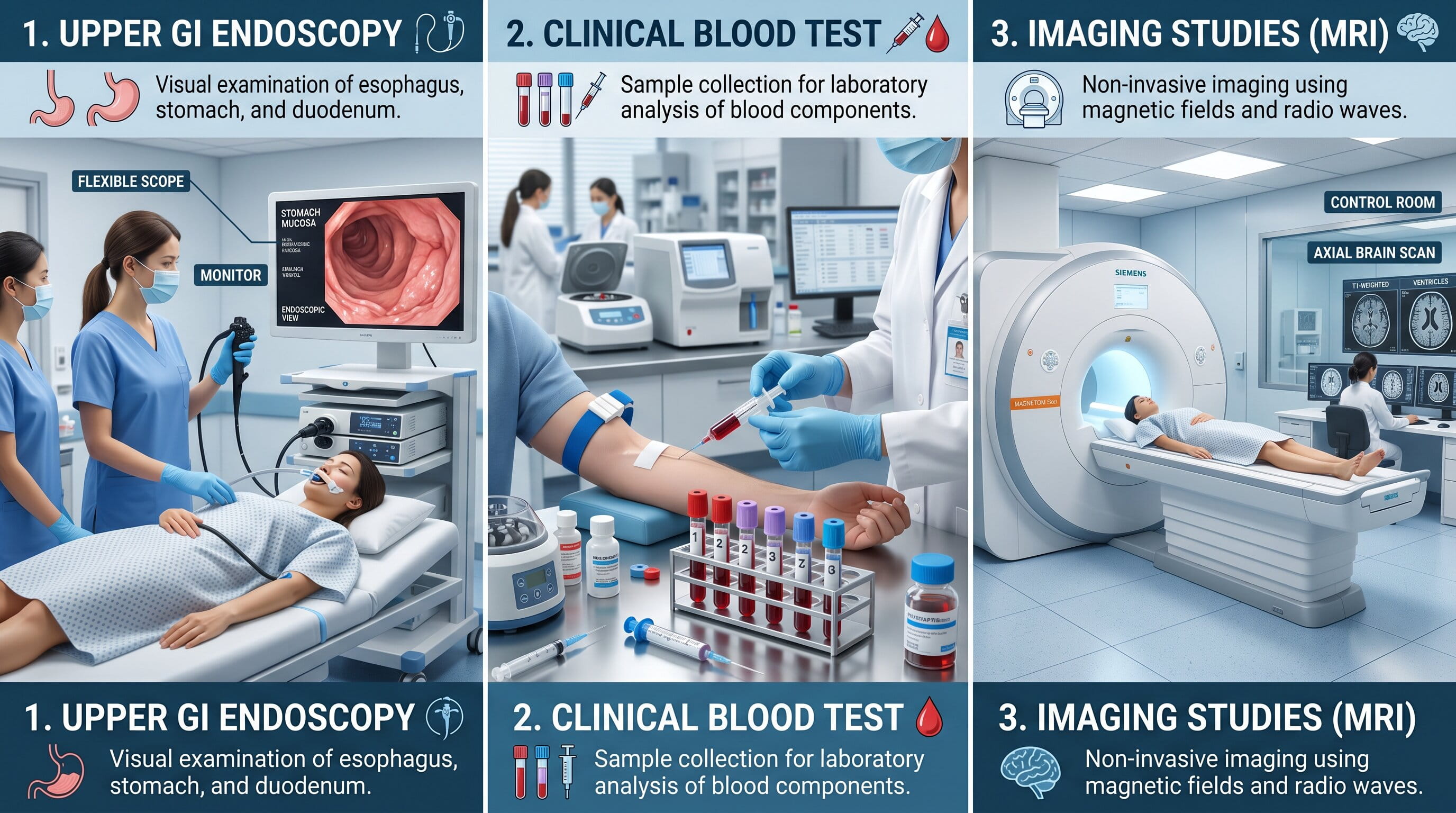
Once the patient is stabilized, the doctor will conduct tests to identify the cause of the bleeding. These tests may include:
An upper GI endoscopy (esophagogastroduodenoscopy) is the most common diagnostic tool for identifying the source of bleeding. During this procedure, a flexible tube with a camera is inserted through the mouth to visualize the esophagus, stomach, and duodenum. It allows doctors to pinpoint the cause of bleeding, whether it’s an ulcer, varices, or a tumor.
Blood tests will be performed to assess the extent of blood loss and check for signs of anemia (low red blood cell count) or liver damage (in the case of cirrhosis or esophageal varices).
If the cause of bleeding cannot be determined with an endoscopy, additional imaging studies, such as a CT scan or ultrasound, may be conducted to look for tumors, liver disease, or other underlying conditions that could be contributing to the bleeding.
Once the source of the bleeding has been identified, doctors will determine the most appropriate treatment. Here are the common treatment options for hematemesis:
For bleeding that can be treated directly, endoscopic procedures are often used:
In rare cases where bleeding cannot be controlled through endoscopy or medications, surgery may be required to remove a tumor, treat a large ulcer, or address other underlying causes of hematemesis.
After treatment, the patient will be closely monitored to ensure that bleeding does not recur. Follow-up care may include:
Patients with peptic ulcers will likely be prescribed PPIs or H2 blockers to reduce stomach acid and help the ulcers heal. Antibiotics may also be given if an H. pylori infection is present.
Doctors will advise on lifestyle modifications to prevent further episodes of hematemesis:
Follow-up appointments with a gastroenterologist will be scheduled to monitor healing and prevent further bleeding. For patients with esophageal varices or liver disease, routine endoscopies may be necessary to check for recurrence of bleeding.
Prevention is key in managing hematemesis, particularly for those with ongoing conditions like peptic ulcers or cirrhosis. Some steps to prevent future episodes include:

Experiencing hematemesis can be a terrifying event, but knowing what to expect during the diagnostic and treatment process can help ease anxiety. From stabilization and diagnostics to endoscopic treatments and lifestyle changes, there are multiple steps involved in managing and preventing vomiting blood. With timely intervention and proper care, the risk of complications can be minimized.
Seek medical attention immediately if you vomit blood. Call emergency services if the bleeding is severe or persistent.
In many cases, hematemesis can be treated with medications and endoscopic procedures. Surgery is reserved for more severe cases where other treatments have failed.
The cause of hematemesis is typically determined through an upper GI endoscopy, blood tests, and imaging studies to assess the source of bleeding.
While stress doesn’t directly cause hematemesis, it can worsen conditions like ulcers or gastritis, increasing the risk of bleeding and vomiting blood.
Recovery depends on the underlying cause and severity of bleeding. After treatment, patients will be monitored and may need lifestyle changes to prevent recurrence.