
Vomiting blood, medically known as hematemesis, is a frightening symptom that can occur suddenly. It’s a sign of bleeding in the upper gastrointestinal (GI) tract, which includes the esophagus, stomach, and duodenum. Vomiting blood is often a medical emergency, and it’s crucial to understand its potential causes and seek prompt medical attention.
While vomiting blood can be a sign of relatively mild conditions, it’s also associated with life-threatening diseases. In this blog, we’ll explore what it means when you vomit blood, the most common causes of hematemesis, and what you should do if it happens.
Hematemesis is the medical term for vomiting blood. The appearance of the blood can give doctors important clues about where the bleeding is coming from in the GI tract:
Hematemesis is a serious condition that requires immediate medical evaluation. If you vomit a significant amount of blood or if it’s accompanied by symptoms like dizziness, rapid heartbeat, or severe abdominal pain, seek emergency care right away.
There are many conditions that can cause hematemesis. Some are more serious than others, but they all require medical attention. Here are some of the most common causes:
Peptic ulcers are open sores that develop in the lining of the stomach or duodenum. They occur when stomach acid erodes the protective lining, allowing the acid to irritate the underlying tissue. This can lead to bleeding, resulting in the vomiting of blood.
Peptic ulcers are most commonly caused by:
Esophageal varices are enlarged veins in the lower part of the esophagus, often caused by liver cirrhosis. When the liver becomes damaged, it increases pressure in the veins that carry blood to the liver, which can cause the veins in the esophagus to swell. These varices can rupture and bleed, leading to hematemesis.
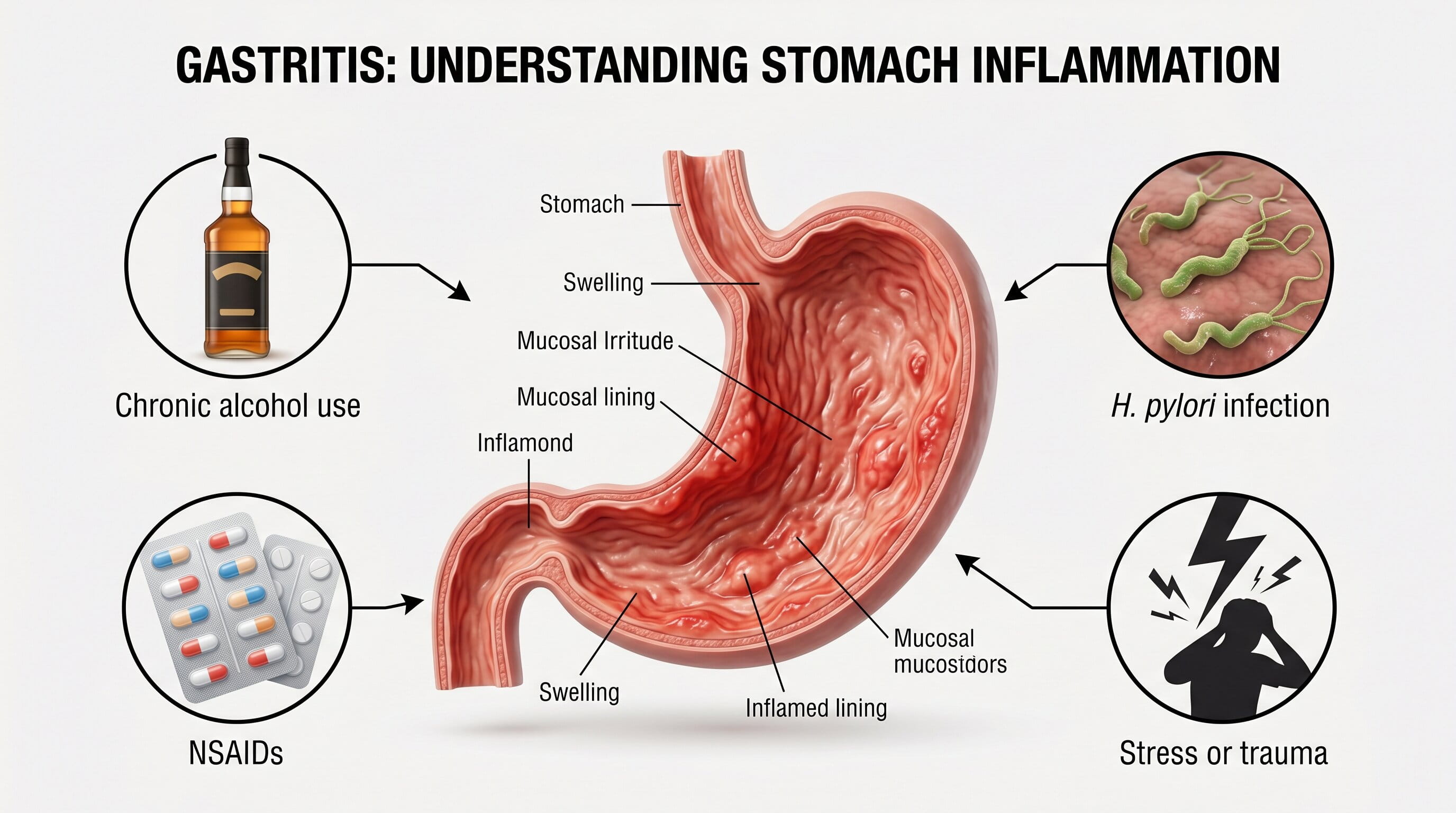
Gastritis refers to the inflammation of the stomach lining, often caused by:
If the stomach lining is inflamed for a prolonged period, it can lead to erosive gastritis, where the tissue breaks down and bleeds, resulting in vomiting blood.
A Mallory-Weiss tear is a tear in the mucous membrane where the esophagus meets the stomach. These tears are typically caused by severe vomiting or retching, often after heavy drinking. When the tear occurs, it can lead to bleeding and hematemesis.
Certain types of gastrointestinal cancers, such as stomach cancer or esophageal cancer, can cause hematemesis. Tumors may bleed into the stomach or esophagus, leading to vomiting blood.
Though less common, hematemesis can also result from other conditions, including:
If you experience hematemesis, you should seek medical attention immediately, especially if:
Even if you are not sure about the severity of the bleeding, it’s always better to seek prompt medical care, as some causes of hematemesis can be life-threatening if not treated immediately.
The diagnosis of hematemesis involves several tests and procedures to determine the source of the bleeding:
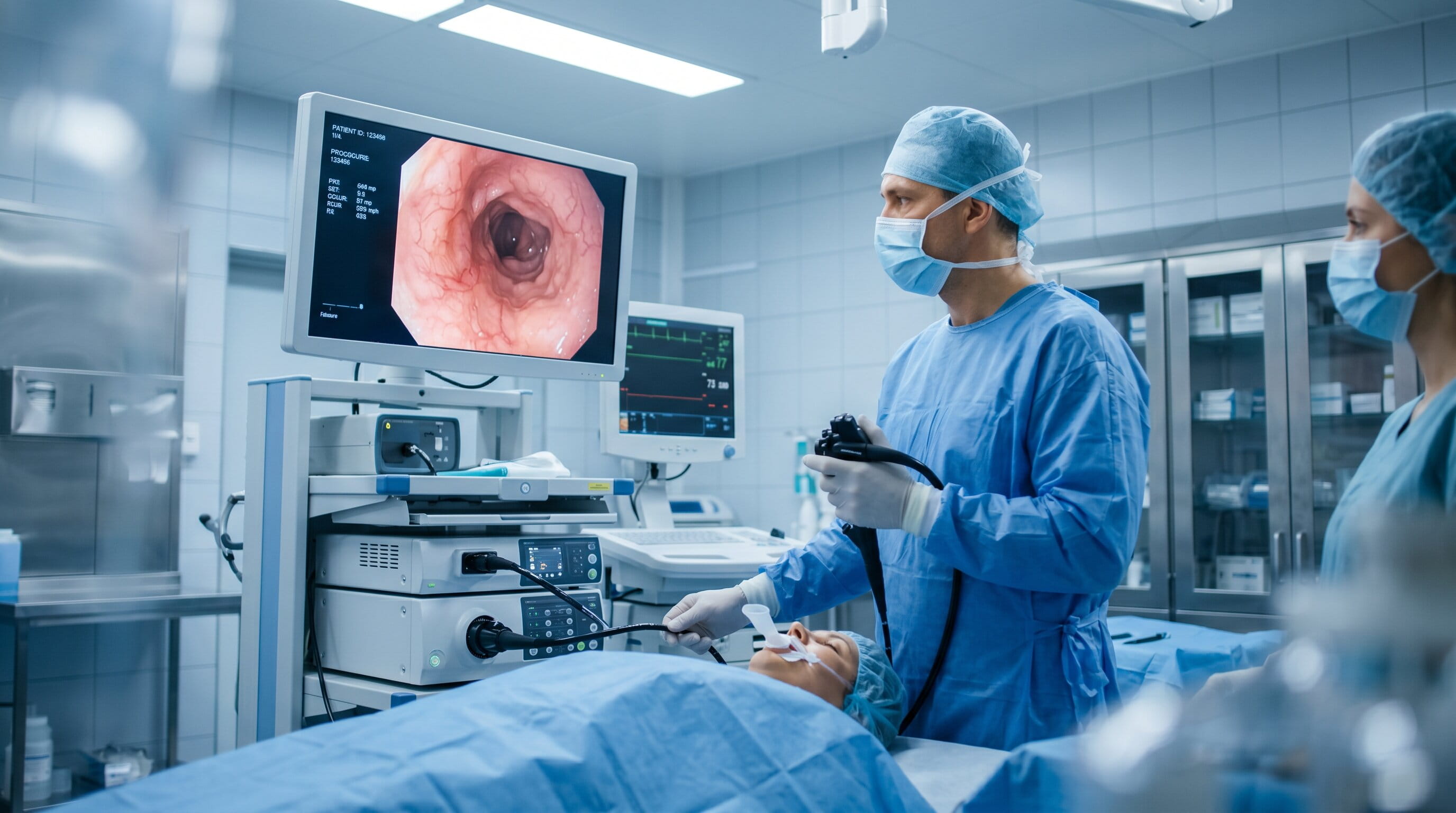
Endoscopy is the most common method for identifying the cause of hematemesis. During this procedure, a flexible tube with a camera is inserted into the esophagus, stomach, and duodenum. The doctor can directly visualize any ulcers, varices, or other issues causing the bleeding.
Blood tests help determine the extent of blood loss and assess whether you have anemia (low red blood cell count). These tests also check for liver function and signs of infection.
In some cases, additional imaging tests, like a CT scan or ultrasound, may be used to check for conditions like liver disease or tumors in the GI tract.
Treatment of hematemesis depends on the underlying cause of the bleeding. The primary goal is to stabilize the patient and stop the bleeding.
In severe cases where bleeding cannot be controlled with medication or endoscopic treatments, surgery may be required to address the underlying condition.
Vomiting blood is a serious symptom that requires immediate medical attention. While it can be caused by several conditions, most of which are treatable, it’s important to understand the potential causes and seek prompt care. With early intervention, the majority of people who experience hematemesis can recover without long-term complications.
Hematemesis is often caused by conditions like peptic ulcers, gastritis, esophageal varices, and gastrointestinal cancer. It can also result from Mallory-Weiss tears or less common causes like angiodysplasia or AVMs.
Preventing hematemesis involves avoiding excessive alcohol, managing NSAID use, quitting smoking, and maintaining a healthy diet. Regular checkups for conditions like liver disease and ulcers can also help prevent GI bleeding.
While gastrointestinal cancers can cause hematemesis, they are less common than other causes like ulcers or varices. It’s important to get an accurate diagnosis to determine the cause.
Seek emergency medical attention if you vomit blood, especially if it’s a large amount or accompanied by other symptoms like dizziness or severe abdominal pain.
Treatment involves stabilizing the patient, identifying the source of bleeding, and stopping the bleeding. This may include medications, endoscopic procedures, or surgery, depending on the underlying cause.