Hematemesis refers to vomiting blood, which is typically a sign of bleeding in the upper gastrointestinal (GI) tract, including the esophagus, stomach, or duodenum. It is an alarming symptom that often indicates a serious condition, and should never be ignored. Vomiting blood can vary in appearance; it might appear as bright red blood or dark, coffee-ground-like material depending on how long the blood has been in the stomach.
While the sight of blood may immediately cause panic, it’s important to understand that not all cases of hematemesis are equally severe. The source of the bleeding, the volume of blood lost, and the patient's overall health all influence the seriousness of the condition. In this article, we’ll explore what hematemesis is, its common causes, when it becomes an emergency, and how it is treated.

What Causes Hematemesis?
Hematemesis can arise from a variety of conditions affecting the upper GI tract. The blood is typically coming from the esophagus, stomach, or duodenum, and the causes can range from common and treatable conditions to more serious, life-threatening ones. Let’s break down the most common causes:
1. Peptic Ulcers
Peptic ulcers are sores that develop in the lining of the stomach or the duodenum (the first part of the small intestine). These ulcers are often caused by infection with the bacteria Helicobacter pylori or by the long-term use of nonsteroidal anti-inflammatory drugs (NSAIDs). When the ulcer erodes into blood vessels, it can lead to bleeding, which may present as hematemesis.
Symptoms and Diagnosis:
People with peptic ulcers often experience burning stomach pain, nausea, and indigestion. The diagnosis is usually made through an endoscopy, where a doctor looks at the ulcer and assesses its severity.
Treatment:
Treatment includes proton pump inhibitors (PPIs) or H2 blockers to reduce stomach acid, antibiotics to treat H. pylori, and avoiding NSAIDs. In more severe cases, endoscopic procedures or surgery may be required.
2. Esophageal Varices
Esophageal varices are enlarged veins in the esophagus that develop when there is high blood pressure in the portal vein, typically due to liver disease. The most common cause is cirrhosis, which causes scarring of the liver tissue. These varices can rupture and lead to severe bleeding, resulting in hematemesis.
Symptoms and Diagnosis:
Signs of esophageal varices often include difficulty swallowing, fatigue, and jaundice (yellowing of the skin). An endoscopy can identify varices, and treatment focuses on managing the underlying liver disease and preventing bleeding.
Treatment:
To prevent bleeding, patients may be given beta-blockers to reduce portal pressure. If varices do rupture, endoscopic banding or sclerotherapy (injecting a solution to shrink the varices) is used. In some cases, surgery or a liver transplant may be needed.
3. Gastritis
Gastritis is inflammation of the stomach lining, often caused by excessive alcohol use, stress, certain medications (like NSAIDs), or bacterial infections, particularly H. pylori. Chronic gastritis can lead to erosions in the stomach lining, resulting in bleeding.
Symptoms and Diagnosis:
Symptoms may include nausea, abdominal pain, indigestion, and loss of appetite. A diagnosis can be made via blood tests, stool tests, or endoscopy.
Treatment:
Treatment involves proton pump inhibitors (PPIs) or H2 blockers to reduce stomach acid, and antibiotics if an H. pylori infection is present. Avoiding alcohol and NSAIDs is also crucial.
4. Mallory-Weiss Tear
A Mallory-Weiss tear is a tear in the mucous membrane at the junction between the stomach and esophagus. This is usually caused by severe vomiting or retching, which places strain on the stomach lining. The tear can result in significant bleeding, leading to hematemesis.
Symptoms and Diagnosis:
The most common symptom is vomiting blood after a bout of forceful vomiting. An endoscopy is used to visualize the tear and determine the severity of the injury.
Treatment:
In most cases, Mallory-Weiss tears heal on their own with conservative management, including rest and antiemetic medications. Severe tears may require endoscopic treatment to stop the bleeding.
5. Gastric Cancer
Gastric cancer, or stomach cancer, is a less common but more serious cause of hematemesis. The tumor may erode into blood vessels, causing bleeding that presents as hematemesis.
Symptoms and Diagnosis:
Symptoms often include unexplained weight loss, nausea, early satiety (feeling full after eating only a small amount), and abdominal pain. A diagnosis is typically made through endoscopy, biopsy, and imaging studies.
Treatment:
Treatment options include surgery, chemotherapy, radiation, and targeted therapies depending on the stage of the cancer.
When Is Hematemesis an Emergency?
Not all cases of hematemesis are equally urgent, but any instance of vomiting blood should be evaluated by a healthcare professional. It becomes an emergency when the following factors are present:
- Volume of Blood: If the person is vomiting large amounts of blood, it can lead to shock or life-threatening complications.
- Signs of Shock: Symptoms of shock, such as rapid heart rate, low blood pressure, dizziness, fainting, and confusion, require immediate intervention.
- Severe Pain: If the hematemesis is accompanied by severe abdominal pain or chest pain, immediate medical attention is necessary.
- Chronic Conditions: In people with known liver disease or ulcers, vomiting blood is more likely to be a sign of a severe complication.
If you or someone you know is experiencing hematemesis, it is critical to seek emergency medical attention, especially if the vomiting continues, the blood appears dark, or there are signs of shock.
How Hematemesis is Diagnosed
Diagnosing hematemesis involves identifying the underlying cause of the bleeding. The following diagnostic tests are typically performed:
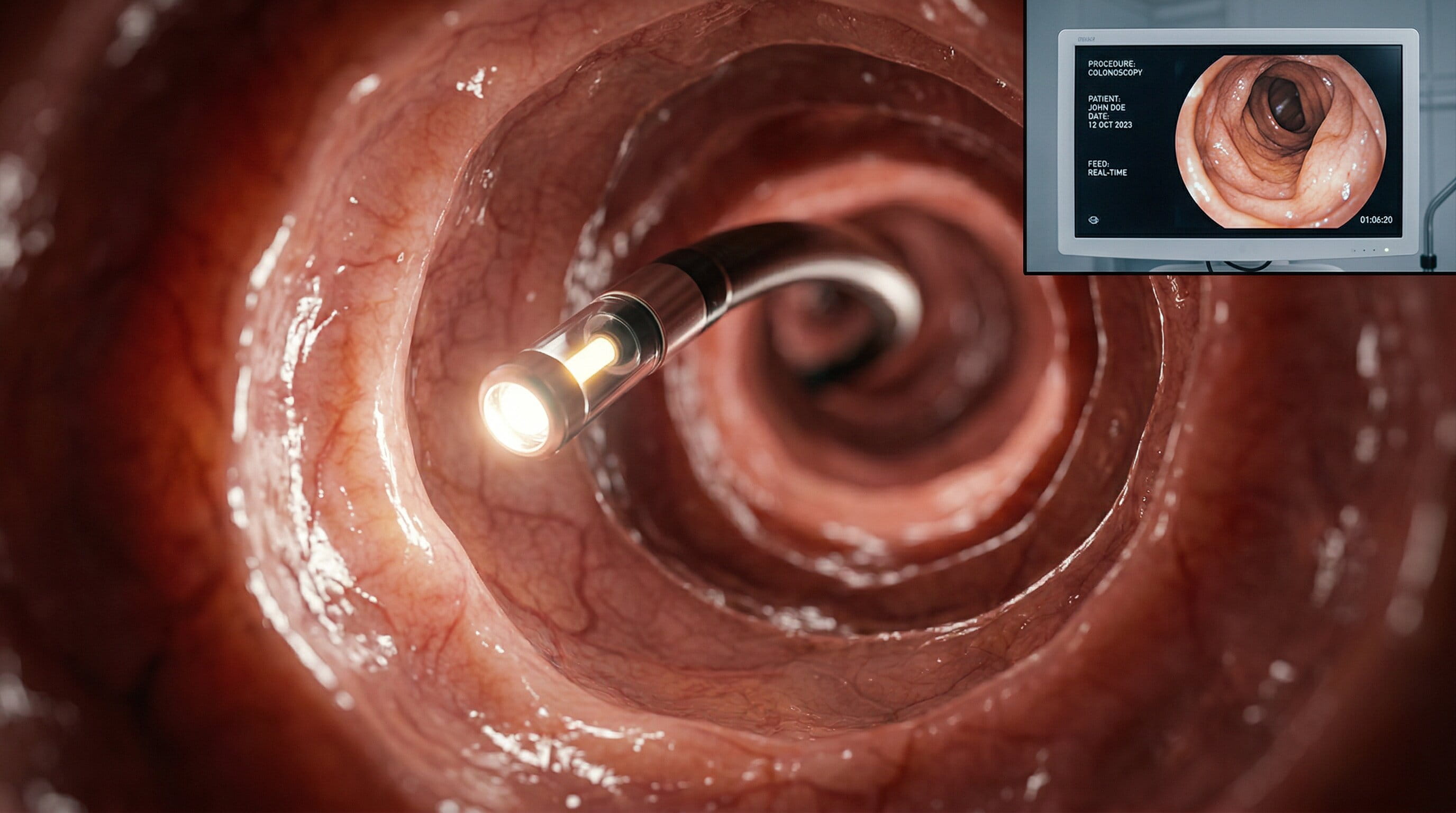
1. Endoscopy
Endoscopy is the most common diagnostic tool. A flexible tube with a camera is inserted through the mouth to examine the esophagus, stomach, and duodenum. It allows doctors to visually identify the source of the bleeding and, in some cases, stop the bleeding via cauterization or banding.
2. Blood Tests
Blood tests can help determine the severity of blood loss, check for anemia, and assess liver function. In cases of suspected infection, blood cultures may also be taken.
3. Imaging
In certain cases, imaging studies like a CT scan may be used to identify sources of bleeding that are not visible on endoscopy.
Treatment for Hematemesis
Treatment for hematemesis depends on the cause and severity of the bleeding. It may range from conservative care to emergency procedures.
1. Conservative Treatment
For mild cases, doctors may recommend medications like proton pump inhibitors (PPIs) or H2 blockers to reduce stomach acid and help the body heal. Rest, hydration, and monitoring may also be part of the treatment plan.
2. Endoscopic Procedures
If the bleeding is more severe, endoscopic treatment can help. Procedures like banding or sclerotherapy are used to stop bleeding from varices or ulcers. Cauterization may also be used to seal blood vessels.
3. Surgery
In rare cases, when the bleeding is severe and cannot be controlled with medications or endoscopy, surgery may be needed. Surgery is also necessary for certain conditions, such as gastric cancer or large ulcers.
4. Blood Transfusions
For patients who have lost a significant amount of blood, blood transfusions may be required to restore blood volume and stabilize the patient.
Conclusion
Hematemesis is a serious condition that requires immediate medical attention. It can be caused by a variety of conditions, ranging from peptic ulcers to esophageal varices to cancer. While some cases may be treated conservatively, others require more intensive intervention, such as endoscopy or surgery.
If you experience hematemesis, it is crucial to seek medical help immediately, especially if there are signs of shock, severe pain, or a significant volume of blood. Early detection and treatment are key to preventing complications and ensuring the best possible outcome.




