
Hematemesis refers to the vomiting of blood and is a potentially serious symptom of gastrointestinal (GI) bleeding. The blood can be bright red or appear as coffee-ground material depending on how long it has been in the stomach. Hematemesis requires immediate medical attention to identify the underlying cause and prevent complications.
When a patient presents with hematemesis, the first step is always to stabilize the person, especially if they have lost a significant amount of blood. Once the patient is stabilized, doctors will work to identify the cause of the bleeding. This process often involves a combination of medical history, physical examination, and diagnostic tests.
Several diagnostic tests and procedures are used to determine the cause of hematemesis, identify the source of bleeding, and assess the severity of the situation. Here’s a breakdown of the most common tests and their purposes:
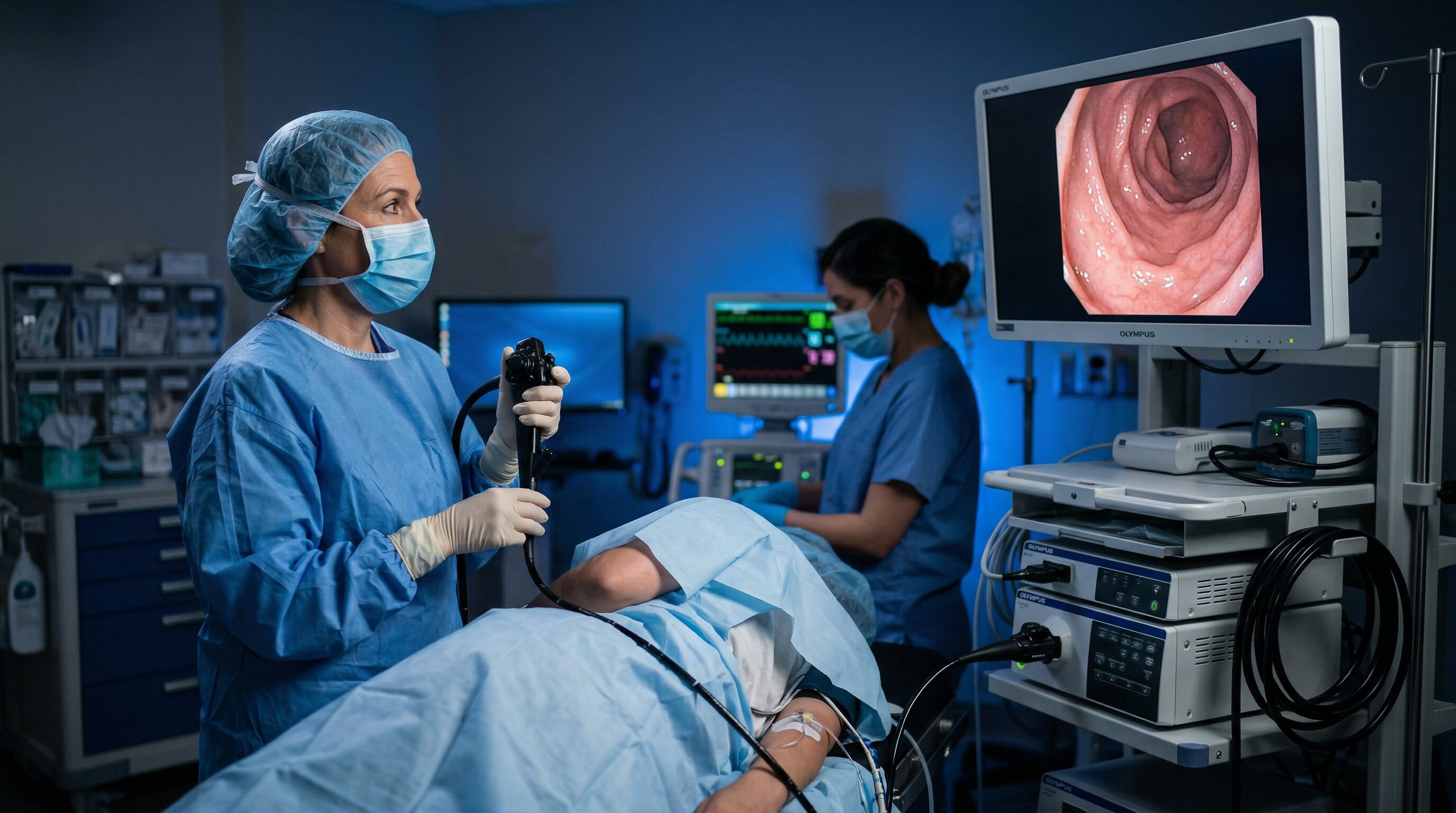
Endoscopy is the primary test used to diagnose the cause of hematemesis. It involves inserting a long, flexible tube with a camera (an endoscope) through the mouth to examine the esophagus, stomach, and duodenum. The procedure allows doctors to visually identify the source of bleeding, such as:
Endoscopy can also be used to treat the bleeding in some cases, such as banding esophageal varices or cauterizing bleeding ulcers.
Blood tests help doctors assess the severity of blood loss and the patient’s overall health. Key tests include:
These tests can help identify whether the bleeding is due to an underlying condition such as liver disease, ulcers, or a clotting disorder.
In some cases, imaging studies may be required to identify the source of bleeding, particularly when an endoscopy is inconclusive. Common imaging techniques include:
In some cases, stool tests may be performed to check for the presence of blood in the stool, even if hematemesis has not occurred. The fecal occult blood test (FOBT) is commonly used to detect hidden blood in the stool. While this test cannot diagnose the exact cause of hematemesis, it can help detect bleeding from the lower GI tract or other sources.
In rare cases, if the source of bleeding is unclear, doctors may use gastric lavage. This involves flushing the stomach with a saline solution to remove any remaining blood, which can help doctors identify the source more easily through subsequent endoscopy or imaging.
In some cases, further tests may be required to understand the cause of hematemesis. These could include tests like CT angiography or capsule endoscopy if the bleeding source remains elusive after initial testing. Doctors may also recommend repeat endoscopies to monitor for recurrent bleeding.
Once the cause of hematemesis has been diagnosed, treatment focuses on addressing the underlying condition. For example:

If you experience hematemesis, it is crucial to seek medical help immediately, especially if any of the following signs are present:
Hematemesis is a serious condition that requires quick identification and intervention. Understanding the diagnostic tests involved in diagnosing the cause of hematemesis can help both patients and healthcare professionals navigate the situation more effectively. Early diagnosis, followed by appropriate treatment, is key to managing this life-threatening symptom and addressing its underlying causes.
Hematemesis is the medical term for vomiting blood. It can appear as bright red blood or dark, coffee-ground-like material, depending on how long the blood has been in the stomach.
Common causes include peptic ulcers, esophageal varices, gastritis, Mallory-Weiss tears, and stomach cancer. It may also result from bleeding disorders or liver disease.
Diagnosis involves a physical exam, blood tests, endoscopy (upper GI), and imaging studies like CT scans. A doctor may also use stool tests to detect hidden blood.
If you vomit blood, seek medical attention immediately. Call emergency services if you experience significant bleeding, signs of shock, or severe pain.
Yes, treatment depends on the underlying cause. It may include medications to reduce stomach acid, endoscopic procedures to stop bleeding, or surgery in severe cases.
Not always, but it should always be treated seriously. Large amounts of blood, ongoing bleeding, or signs of shock require immediate emergency care.