
Hematemesis, or vomiting blood, is a concerning symptom that indicates bleeding in the upper gastrointestinal (GI) tract. Since it can be caused by various conditions, including peptic ulcers, esophageal varices, and gastritis, it is important to identify the exact source of bleeding to determine the appropriate treatment.
One of the most effective diagnostic tools for identifying the cause of hematemesis is endoscopy. This procedure allows doctors to directly visualize the esophagus, stomach, and duodenum, providing valuable insight into the source of bleeding and enabling targeted treatment. In this blog, we’ll explore the role of endoscopy in the diagnosis of hematemesis, how it works, and its benefits and limitations.
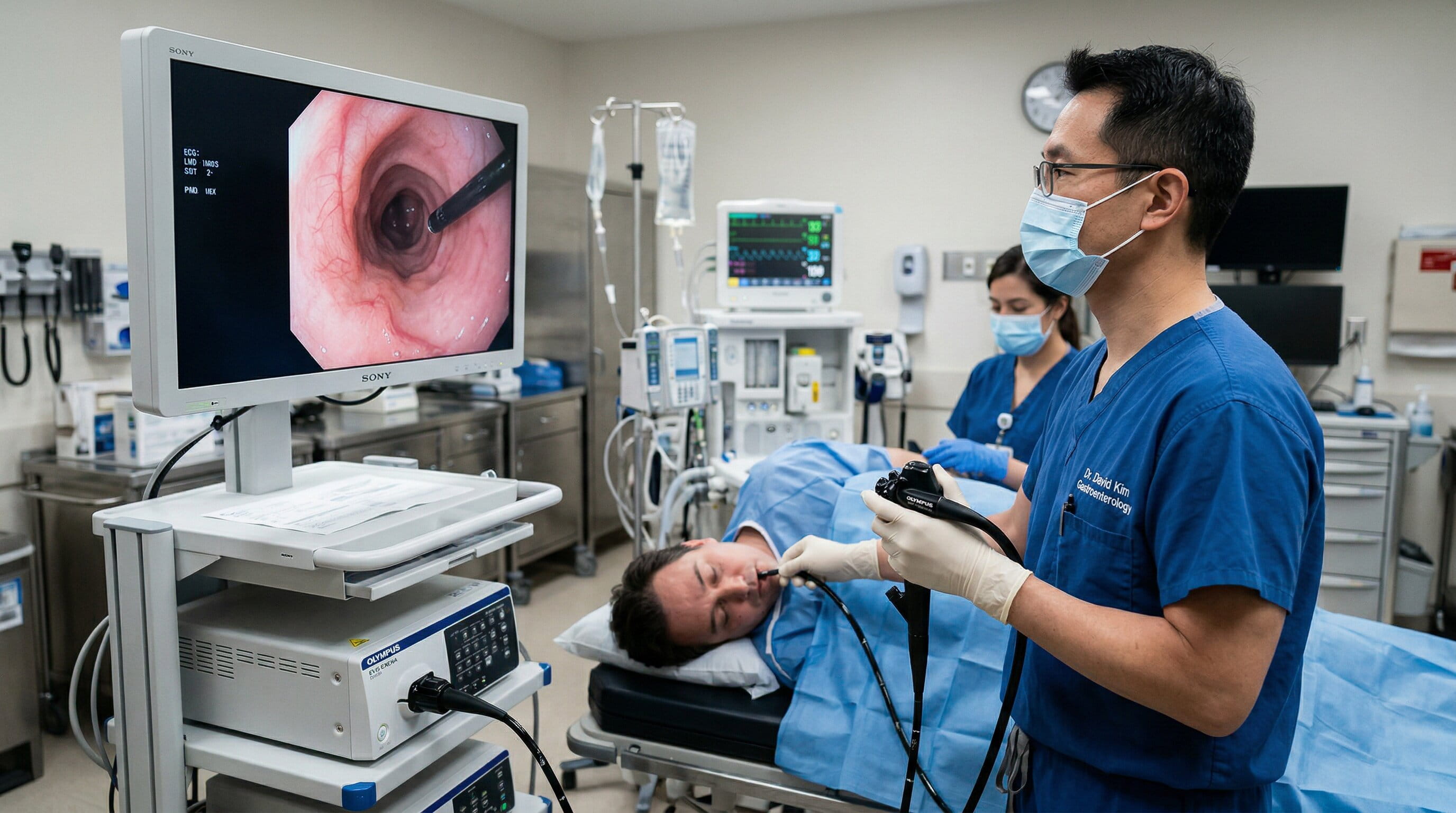
Endoscopy is a medical procedure that involves the use of a flexible tube with a light and camera (an endoscope) to examine the inside of the body. When used to investigate hematemesis, the endoscope is inserted through the mouth and advanced down the throat into the upper GI tract. This allows doctors to view the esophagus, stomach, and duodenum, which are the primary areas where bleeding typically originates in cases of hematemesis.
Endoscopy is a minimally invasive procedure, meaning that it doesn’t require large incisions or surgery. It provides real-time images of the GI tract and is crucial for identifying conditions like ulcers, varices, and tears that can cause bleeding. Additionally, endoscopy can be used to treat some causes of bleeding, making it both a diagnostic and therapeutic tool.
Endoscopy is essential for determining the exact cause of hematemesis. Here’s how it contributes to the diagnosis:
The primary role of endoscopy in hematemesis diagnosis is to visualize the source of the bleeding. Common conditions that can cause blood to be vomited include:
By using the endoscope to directly examine the upper GI tract, doctors can identify these conditions and pinpoint the exact location of the bleeding, allowing for more accurate treatment.
In addition to identifying the source, endoscopy helps assess the severity of the bleeding. Some conditions may cause minor bleeding, while others may lead to life-threatening hemorrhages. The doctor can determine how much blood is present in the GI tract and whether immediate intervention is required. For example, if esophageal varices are found, doctors can assess whether they are actively bleeding or at risk of bleeding.
In some cases, endoscopy can be used to perform a biopsy, where small tissue samples are taken from the lining of the stomach, esophagus, or duodenum. This is important when there is suspicion of cancer or other abnormal tissue growths. A biopsy helps determine whether the cause of hematemesis is related to a tumor or a benign condition.
One of the key advantages of endoscopy is that it allows doctors to treat certain causes of bleeding immediately. For instance:
This ability to treat and diagnose in the same procedure can be lifesaving in severe cases of hematemesis.
Endoscopy is widely used due to its many benefits in diagnosing and managing hematemesis. These advantages include:
Endoscopy is minimally invasive, meaning it does not require large incisions or major surgery. This reduces the risk of infection and speeds up recovery time compared to surgical options.
The ability to see the source of bleeding in real time allows doctors to make immediate treatment decisions. This is especially crucial in cases where rapid intervention is needed, such as with esophageal varices or massive gastric bleeding.
Endoscopy serves both diagnostic and therapeutic purposes. In many cases, the same procedure can be used to treat the underlying cause of bleeding, reducing the need for additional surgeries or treatments.
Endoscopy is highly accurate in diagnosing the source of bleeding. It is especially useful in distinguishing between different types of gastrointestinal conditions, such as ulcers, tumors, and varices.
While endoscopy is a highly effective tool, it does have some limitations, including:
Endoscopy can only visualize the upper GI tract (esophagus, stomach, and duodenum). If the source of bleeding is in the lower GI tract, such as the colon or rectum, a colonoscopy or other diagnostic tools will be required.
Although endoscopy is minimally invasive, it still requires sedation or anesthesia for patient comfort. There is also a small risk of complications, such as perforation or infection, though these are rare.
The success of the procedure depends on the skill and experience of the endoscopist. Misinterpretation or failure to detect subtle signs of bleeding can occur if the endoscopist is inexperienced.
In critically ill patients or those with severe GI bleeding, endoscopy may be challenging or impossible to perform. In these cases, other imaging methods or surgical intervention may be required.

Endoscopy is typically used when the cause of hematemesis is unclear or when other diagnostic tests are inconclusive. Here are some scenarios when endoscopy is commonly used:
Endoscopy plays a critical role in diagnosing and managing hematemesis by directly visualizing the source of bleeding in the upper gastrointestinal tract. It offers several advantages, including its minimally invasive nature, real-time visualization, and the ability to treat certain conditions immediately. While endoscopy is highly effective, it also has limitations that require careful consideration by medical professionals.
If you experience hematemesis, an endoscopy may be necessary to identify the underlying cause of the bleeding and determine the appropriate treatment. Prompt diagnosis and intervention are crucial to managing this serious symptom and preventing further complications.
Endoscopy allows doctors to directly visualize the esophagus, stomach, and duodenum to identify the source of bleeding. It is also used to perform treatments, such as banding or cauterization, to stop active bleeding.
Endoscopy is typically not painful as it is performed under sedation or anesthesia. Patients may experience mild discomfort after the procedure, such as a sore throat.
Endoscopy is highly effective for diagnosing upper GI tract conditions like ulcers, varices, and gastritis. However, it cannot visualize the lower GI tract or other non-GI causes of bleeding.
An endoscopy usually takes between 15 and 30 minutes, depending on the complexity of the procedure. Patients are typically monitored for an additional period as the sedation wears off.
While rare, risks of endoscopy include perforation (tearing of the GI tract), infection, and bleeding. These complications are generally uncommon and can be managed effectively by skilled professionals.