If you live in Jersey Village, TX, or the surrounding Houston area and suffer from ulcerative colitis, you may have noticed mucus in your stool. While it can be an unsettling symptom, it’s important to understand why this happens and what it means for your digestive health. In this blog, we’ll explore what mucus in stool is, why it appears in people with ulcerative colitis, and how you can manage it effectively. We will also provide insights into when you should seek medical attention and how to live well with this condition in Jersey Village, TX
Mucus is a thick, gel-like substance that is naturally produced by the lining of your intestines. It plays a crucial role in protecting the digestive tract by lubricating the intestines and helping move waste through the colon. In a healthy digestive system, mucus is typically present in small amounts, but its presence is not usually noticeable.
However, for individuals with ulcerative colitis (UC), an inflammatory bowel disease (IBD), mucus production can increase significantly. This results in the presence of mucus in the stool, which may be visible to you when you go to the bathroom.
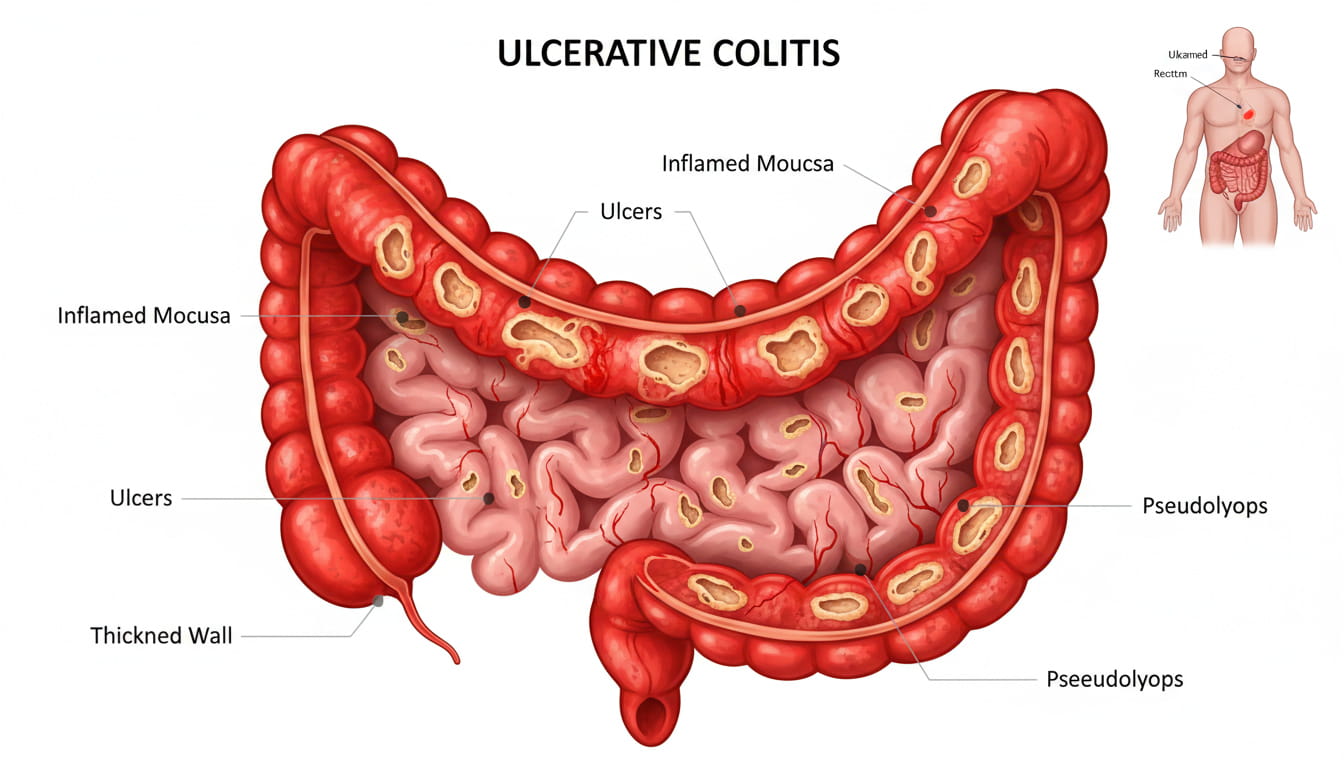
Ulcerative colitis causes inflammation and sores (ulcers) in the inner lining of the colon and rectum. These sores can lead to an overproduction of mucus as the body tries to protect itself from the irritation caused by the inflammation. The increased mucus production is the body’s way of attempting to heal and protect the colon, but it can result in noticeable mucus in the stool.
The mucus is produced by the cells that line the colon, particularly in response to the inflammation. When UC flares up, the mucus may become more prominent, and you may notice it in your stool. Mucus in stool can be clear, white, or even yellowish, depending on the severity of the inflammation and your diet.
For patients in Jersey Village, TX, who are living with ulcerative colitis, understanding how mucus in stool relates to flare-ups is critical. A flare-up is a period of time when the symptoms of UC worsen. During a flare, the colon becomes more inflamed, leading to an increased production of mucus. This can make the mucus more noticeable in your stool.

During flares, it’s common for people to experience other symptoms such as:
Mucus in stool is not always a sign of a flare, but it is more likely to occur during one. Monitoring your symptoms, including the presence of mucus, can help you and your healthcare provider determine the severity of your UC and adjust your treatment plan accordingly.
Mucus in stool is a normal occurrence for people with ulcerative colitis. It’s part of the body’s natural response to inflammation in the intestines. However, the amount of mucus and how often it appears can vary depending on several factors, including the stage of your UC, your diet, and how well you’re managing the condition.
In some cases, mucus in stool may be the only symptom of UC, while in others, it may accompany other signs like diarrhea or abdominal pain. If the mucus is accompanied by blood or severe pain, it could indicate a more serious flare-up that requires medical attention.
Living in Jersey Village, TX, and managing the symptoms of ulcerative colitis, including mucus in stool, can be challenging. Fortunately, there are steps you can take to manage this symptom and improve your quality of life.
The first step in managing mucus in stool is to work with a gastroenterologist who specializes in IBD, like those at GastroDoxs in Jersey Village. Your doctor can help monitor the severity of your ulcerative colitis and provide tailored treatment options to address both inflammation and mucus production.
There are several medications that can help control the inflammation caused by UC, thereby reducing mucus production. Some common medications for UC include:
Working with your doctor, you can determine which medication is right for your specific case.
Dietary changes can also help manage UC symptoms, including mucus in stool. While no one food triggers ulcerative colitis for everyone, many people find that certain foods exacerbate their symptoms. In Jersey Village, TX, you might consider working with a dietitian who specializes in IBD to help create a personalized meal plan.
Here are some general dietary tips:
Dehydration is a concern for people with ulcerative colitis, especially if diarrhea is a frequent symptom. It’s important to drink plenty of fluids throughout the day to stay hydrated. In some cases, electrolyte drinks may also be beneficial to replenish lost minerals.
It can be helpful to keep track of the mucus in your stool, along with other symptoms, in a journal. This can help you and your doctor identify patterns and potential triggers, such as certain foods or stressors, that may contribute to increased mucus production.

While mucus in stool is common for individuals with ulcerative colitis, there are certain signs that should prompt you to seek medical attention immediately. If you experience the following symptoms, it’s important to reach out to a healthcare provider:
In Jersey Village, TX, GastroDoxs offers expert care for those with ulcerative colitis, including diagnostic tests, flare management, and ongoing treatment options.
Ulcerative colitis is a chronic condition, but with the right care and lifestyle modifications, you can live a fulfilling life. In Jersey Village, TX, there are resources available to help you manage your UC effectively. From working with top gastroenterologists to finding local support groups and dietary assistance, living with UC can become more manageable.
If you’re experiencing mucus in stool or other symptoms of ulcerative colitis, don’t hesitate to schedule a consultation with a specialist at GastroDoxs in Jersey Village, TX. We’re here to help you understand your condition, manage symptoms, and improve your quality of life.
Mucus in stool is a common symptom of ulcerative colitis, often caused by inflammation in the colon. It’s part of the body’s natural response to protect the intestines from irritation.
Not always, but it’s more likely to occur during a flare-up. Monitoring other symptoms like abdominal pain and diarrhea can help determine if a flare is present.
Managing UC through medication, diet modifications, and stress reduction can help reduce the amount of mucus in your stool.
Seek medical attention if you notice blood in your stool, experience severe pain, or if the mucus is accompanied by a fever or unexplained weight loss.
Yes, avoiding high-fiber, fatty, and dairy foods during flare-ups can help reduce symptoms like mucus in stool.
Yes, while mucus in stool is common with ulcerative colitis, it can also occur in other gastrointestinal conditions like irritable bowel syndrome (IBS) or infections. Consulting a healthcare provider is essential for an accurate diagnosis.
Some people with ulcerative colitis may still notice small amounts of mucus in their stool even when their condition is in remission. However, a significant increase in mucus could indicate a flare-up.
In addition to mucus, you should look for symptoms like blood in your stool, abdominal pain, frequent diarrhea, or weight loss. These could indicate a flare-up or other complications related to ulcerative colitis.
A gastroenterologist will evaluate the severity of inflammation and may adjust medications, recommend dietary changes, and provide lifestyle tips to manage mucus production and improve overall symptom control.
Yes, stress can exacerbate ulcerative colitis symptoms, including increased mucus production. Managing stress through relaxation techniques, exercise, and proper sleep can help minimize this effect.
Not always. Mucus can sometimes appear during periods of inactivity in ulcerative colitis, especially if the intestines are irritated by factors like diet or medication changes. However, increased mucus could also signal a flare-up.
Ignoring mucus, especially if it’s accompanied by other symptoms like blood or severe pain, can delay the diagnosis of a flare-up or other complications, leading to more serious health issues.
Certain foods can trigger inflammation in the colon, leading to increased mucus production. A low-residue, easy-to-digest diet can help reduce irritation and control symptoms, including mucus in stool.
Yes, medications like aminosalicylates, corticosteroids, and immunosuppressants can help reduce inflammation, which in turn can reduce mucus production in the stool. Your doctor will adjust treatments based on your condition’s severity.
While no natural remedy has been proven to replace medical treatment, some people find that adding probiotics, increasing fiber intake, or drinking herbal teas like peppermint or ginger can support gut health and reduce symptoms.