Health is a major concern in health and majority of the residents in Cypress, TX are not even aware of the risks that their liver is undergoing because of liver complications that are chronic. Cirrhosis is a liver disease that is chronic and results in scarring of the liver tissue. Even though there are numerous causes of cirrhosis, such as alcohol abuse, hepatitis, or fatty liver disease among other causes, one of the most dangerous consequences of cirrhosis is that it directly relates to liver cancer (also known as Hepatocellular carcinoma or HCC). The association between liver cancer and cirrhosis is essential to the inhabitants of Cypress to avert, diagnose, and cure the ailments.
This paper will be discussing cirrhosis, the pathology, the risks it brings as well as how it leads to liver cancer. It will also be listening to the importance of the early detection, lifestyle change and treatment opportunities of the people at risk in Cypress, TX. Because liver disease remains an issue that continues to ruin the lives of several individuals in our society, the information regarding the correlation between cirrhosis and liver cancer could save lives since it encourages early diagnosis and the use of appropriate drugs.
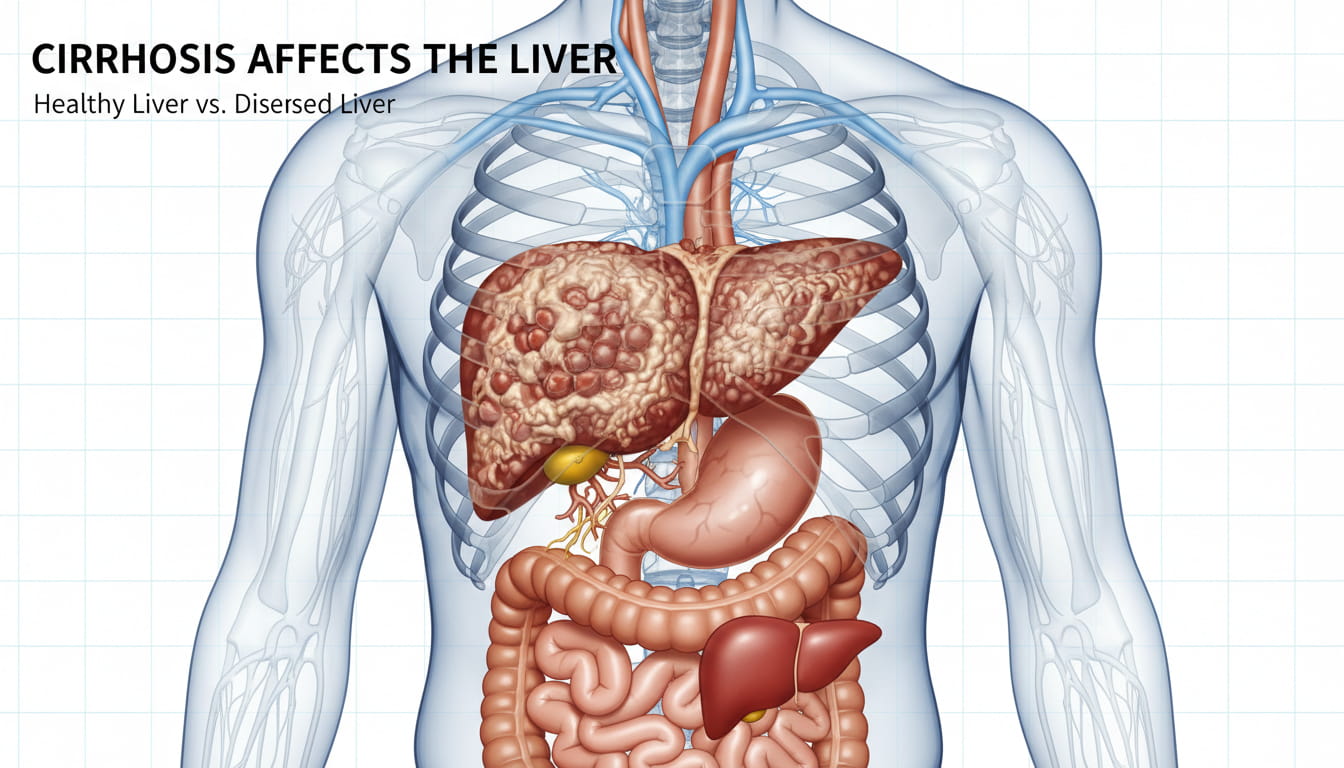
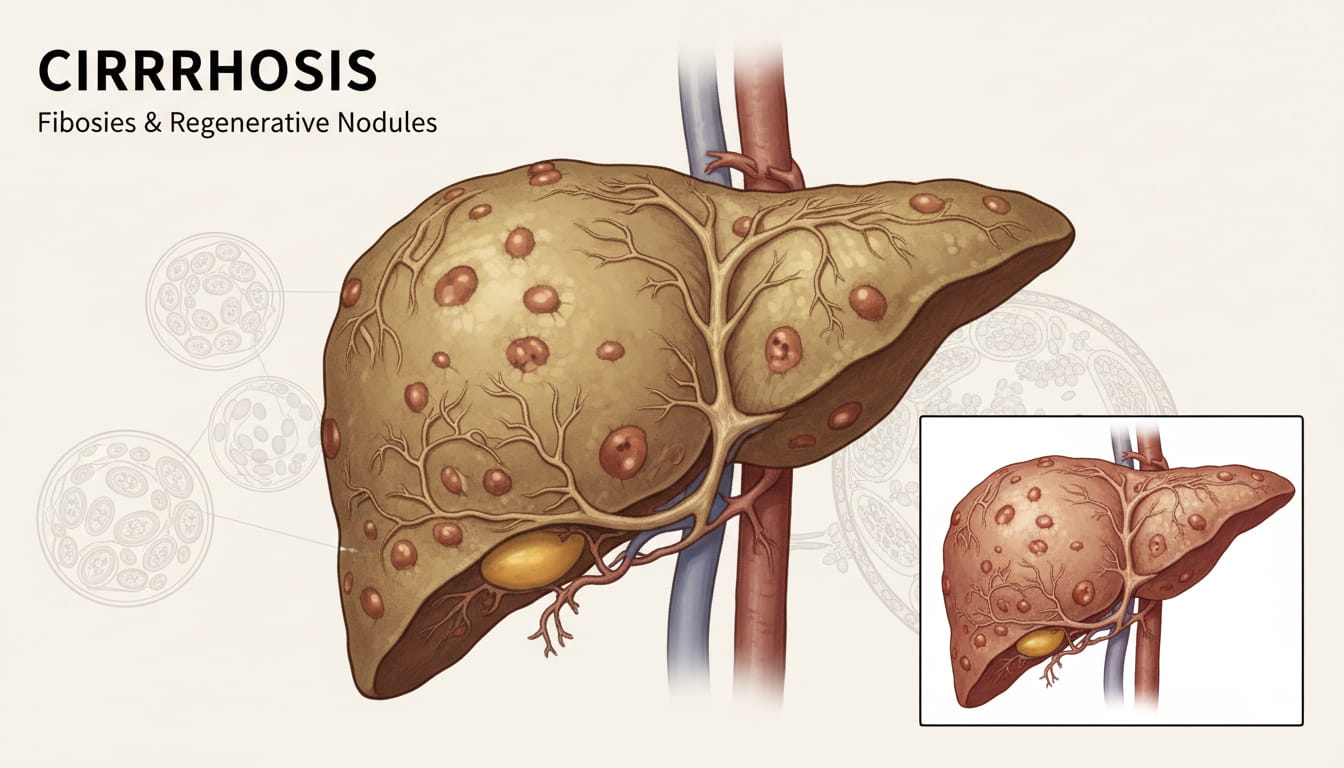
This condition is referred to as cirrhosis in which the liver is scarred a number of times due to persistent liver destruction. Eventually, the liver is destroyed to an extent of not operating well. As the cirrhosis progresses, the liver, which is rather fundamental in metabolism of nutrients, protein synthesis as well as in the removal of toxins, might experience the loss of the functions.
In the first stages of cirrhosis, the liver can compensate the damages and the majority of the patients can not note any visible symptoms. However, as the scarring progresses, it can cause portal hypertension (high blood pressure in the vessels of liver), liver failure and other various complications, such as ascites (fluid build up in the stomach) and bleeding varices (enlarged blood vessels of the esophagus). In addition, cirrhosis is also one of the greatest contributors to predisposing liver cancer especially when the liver is destroyed or inflamed over a long duration of time.
The most alarming consequences of cirrhosis are the fact that it is closely connected to the development of liver cancer. The most common liver cancer is referred to as hepatocellular carcinoma (HCC), and the first complication of cirrhosis. Studies have shown that more than 80 percent of the people who develop hepatocellular carcinoma have had cirrhosis. As the cirrhosis progresses, the liver tissue becomes more scarred, and this situation can allow cancerous cells to develop. Cirrhosis causes liver cancer, and it is the manner in which it does so:
Cirrhosis is a condition that causes the liver to be scarred due to inflammatory damage on the liver. This inflammation continues to destroy the liver cells, and they regenerate continuously. This regeneration and injury process may eventually lead to mutation of liver cells that predisposes individuals to have HCC.
The normal structure of the liver may be destroyed due to the progression of cirrhosis caused by the deposition of scar tissues. This distorted architecture creates spaces where abnormal cells can multiply, which increases the possibility of the development of liver cancer.
Patients with chronic hepatitis B or C are far more susceptible to acquiring cirrhosis, and once cirrhosis is acquired, patients are more at risk of developing liver cancer. The two hepatitis infections cause inflammation and damage of liver cells, and the chronic presence of the two viruses may accelerate the development of cirrhosis, which is another risk factor for liver cancer.
Liver cancer doesn’t develop overnight. The progression from chronic liver disease to cirrhosis, and finally to liver cancer, often occurs over several years or even decades. In people with cirrhosis, the liver becomes increasingly unable to function normally, making it easier for abnormal cells to take hold and multiply. Here are the major risk factors associated with cirrhosis that contribute to the development of liver cancer:
The longer someone has cirrhosis, the higher their risk of developing liver cancer. The severity of cirrhosis also plays a role. Individuals with more advanced liver damage and scarring are at a much higher risk of liver cancer compared to those with mild cirrhosis.
Certain causes of cirrhosis, such as chronic hepatitis and non-alcoholic fatty liver disease (NAFLD), are particularly linked to an increased risk of liver cancer. Hepatitis B and C are known to cause chronic inflammation, increasing the likelihood of liver cancer. NAFLD and non-alcoholic steatohepatitis (NASH) are also emerging as significant risk factors for liver cancer as they can cause fat buildup in the liver, leading to cirrhosis and, eventually, HCC.
Portal hypertension, a condition caused by increased pressure in the veins that carry blood from the intestines to the liver, is common in individuals with cirrhosis. This condition can lead to an environment in which liver cancer can develop, further complicating the disease process.
Early detection of liver cancer is key to improving the prognosis and outcomes for individuals with cirrhosis. Since HCC often develops in cirrhosis patients without causing obvious symptoms until it is advanced, routine screening is essential for those at risk. Early detection through regular monitoring can help ensure the best possible outcome. The following tests are commonly used for early detection:
Regular ultrasound imaging is commonly recommended for individuals with cirrhosis to check for any signs of liver cancer. Ultrasound screenings are effective at detecting tumors in the liver, especially when performed regularly.
Blood tests that measure levels of alpha-fetoprotein (AFP), a substance often elevated in liver cancer, are often used in conjunction with imaging tests to screen for liver cancer. Elevated AFP levels can be an early sign of HCC, but not all liver cancers produce elevated AFP, so regular screenings remain crucial.
More detailed imaging tests, such as CT scans or MRIs, may be used to get a clearer view of the liver and to confirm whether any abnormalities found during ultrasound screenings are cancerous. These tests can also help doctors assess the size and location of any tumors, which is critical for treatment planning.
While there is no cure for cirrhosis, treatment options can help manage the disease and reduce the risk of complications such as liver cancer. If liver cancer is diagnosed, treatment depends on the stage of the cancer and the extent of liver damage. Here are some options for treatment:
For individuals with cirrhosis, lifestyle changes such as avoiding alcohol, maintaining a healthy weight, and controlling diabetes are essential for slowing the progression of the disease. Medications to manage cirrhosis-related complications like portal hypertension or ascites can also help manage the disease.
Liver transplantation may be an option for individuals with end-stage cirrhosis or liver cancer who are not candidates for other treatments. A transplant can provide a healthy liver and improve the quality of life, though eligibility depends on various factors such as age, overall health, and the severity of liver disease.
Surgical resection, or removal of the tumor, may be an option for individuals with early-stage HCC and healthy liver function. In other cases, ablation therapies like radiofrequency ablation (RFA) or transarterial chemoembolization (TACE) may be used to shrink or eliminate tumors without removing the liver.

While it’s not always possible to prevent cirrhosis and liver cancer, residents of Cypress, TX, can take steps to reduce their risk:
Cirrhosis is a serious condition, and its direct link to liver cancer makes it even more critical to detect and manage early. For residents of Cypress, TX, regular screenings, early detection, and lifestyle changes can help reduce the risk of cirrhosis and liver cancer. If you’re at risk, don’t wait for symptoms to appear—schedule a consultation with your gastroenterologist and take the first step toward proactive liver health.
Cirrhosis is the scarring of the liver tissue caused by long-term damage. This scarring disrupts the liver's ability to function properly, affecting critical processes like detoxification and protein production.
Cirrhosis can be caused by chronic alcohol use, hepatitis B or C, NAFLD, or autoimmune diseases. Preventing it involves lifestyle changes like limiting alcohol, managing underlying conditions, and avoiding fatty foods.
Cirrhosis causes chronic liver inflammation and scarring, which increases the risk of developing liver cancer (HCC) due to abnormal cell regeneration and mutations in liver tissue.
Over 80% of liver cancer cases are linked to cirrhosis. People with cirrhosis from hepatitis, alcohol use, or fatty liver disease are at increased risk of developing Hepatocellular carcinoma (HCC).
While Cirrhosis cannot be fully reversed, its progression can be slowed with treatments like medications, lifestyle changes, and regular monitoring. Preventing liver cancer focuses on early intervention.
You can reduce your risk by avoiding excessive alcohol, maintaining a healthy weight, managing diabetes, and regularly screening for hepatitis.
Symptoms include fatigue, unexplained weight loss, abdominal swelling, jaundice, and nausea. Early detection through screening is key to managing Cirrhosis and preventing complications like liver cancer.
Diagnosis typically involves blood tests, imaging tests (like ultrasound or CT scans), and FibroScan for assessing liver stiffness and fibrosis levels. In some cases, a liver biopsy is also recommended.
FibroScan is a non-invasive test that measures liver stiffness, an indicator of liver fibrosis. It is a crucial tool for detecting Cirrhosis and monitoring liver health without the need for a biopsy.
Cirrhosis is classified into four stages based on liver stiffness. The more severe the cirrhosis, the higher the risk of liver cancer. Stage 4 cirrhosis (known as cirrhosis) is most strongly associated with liver cancer.
Treatment for liver cancer in Cirrhosis patients may include surgical resection, liver transplantation, radiation therapy, or transarterial chemoembolization (TACE), depending on the stage of cancer and liver function.
Yes, cirrhosis can lead to complications like ascites (fluid accumulation in the abdomen), variceal bleeding, kidney failure, and hepatic encephalopathy (brain dysfunction due to liver failure).
Regular check-ups with your gastroenterologist in Cypress, TX, are essential. This includes FibroScan tests, blood work, imaging tests, and monitoring for complications to assess how your liver is responding to treatment.
Yes, managing Cirrhosis involves:
Liver transplantation is often the last option for advanced Cirrhosis or liver cancer patients. Candidates must meet specific criteria, including the degree of liver damage and cancer stage, and must undergo evaluation to determine eligibility.