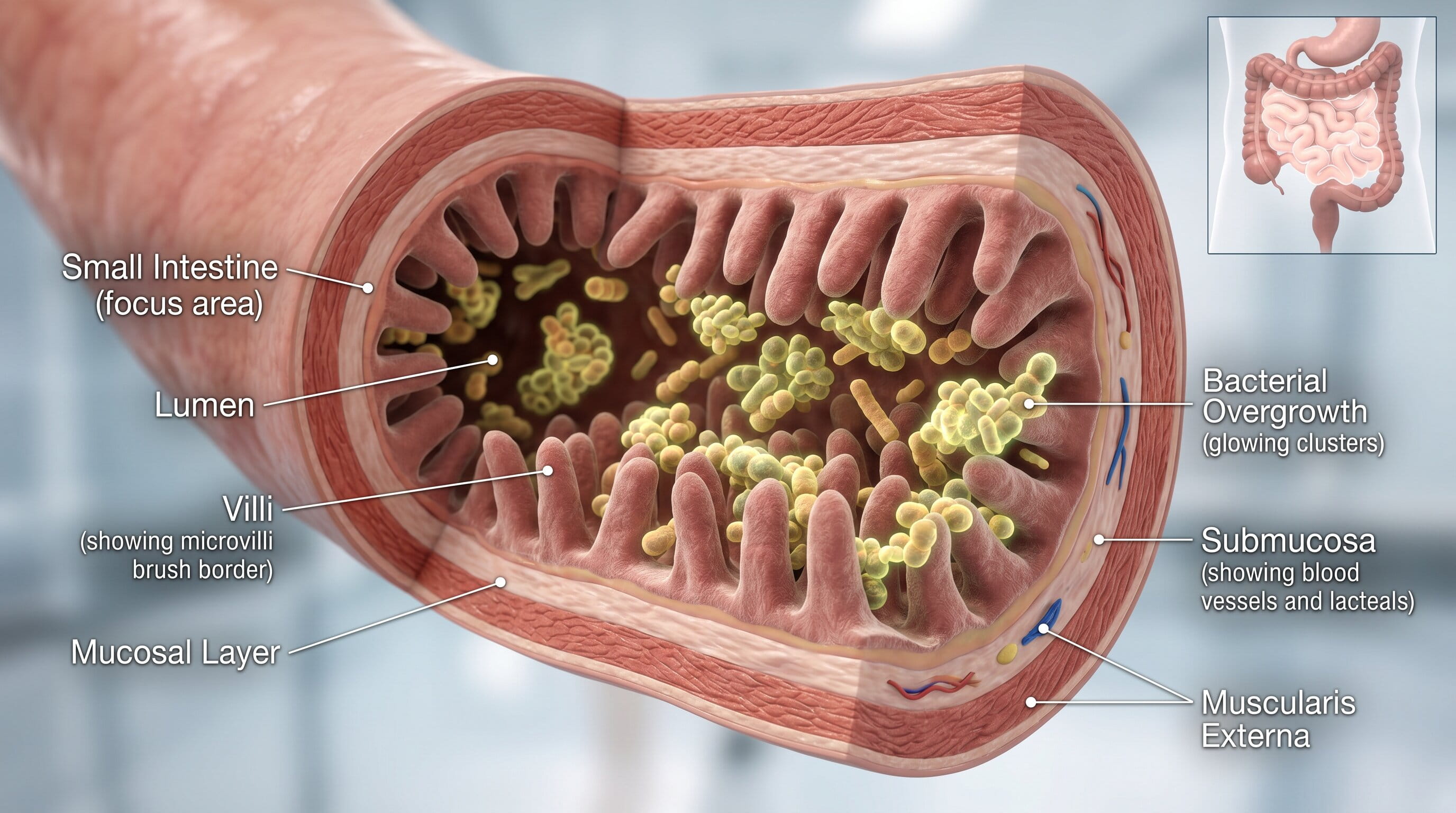
Small Intestinal Bacterial Overgrowth (SIBO) occurs when an abnormal increase of bacteria in the small intestine leads to digestive discomfort. Unlike the large intestine, the small intestine is not designed to house a high concentration of bacteria. This imbalance can lead to symptoms such as bloating, diarrhea, constipation, and nutrient malabsorption.
In the context of SIBO, this overgrowth of bacteria may hinder the natural digestive processes, resulting in improper digestion of food. But what many people don't realize is that this imbalance can also affect mental health through the gut-brain axis.
The gut-brain axis (GBA) refers to the bidirectional communication system between the gut and the brain. This system is essential for regulating emotions, cognition, and mental health, linking the central nervous system (CNS) with the enteric nervous system (ENS). The gut is often referred to as the "second brain" due to the vast number of neurons lining the gastrointestinal tract.
The gut and brain communicate through several mechanisms, including:
When this connection is disrupted, it can lead to a range of mental health symptoms, such as:
The bacteria in the small intestine play a vital role in digestion, but they also influence the production of neurotransmitters, such as serotonin, which is crucial for regulating mood. When SIBO occurs, an overgrowth of bacteria can alter the balance of the microbiome, reducing serotonin production and leading to anxiety and depression.
When bacteria in the small intestine overgrow, they often trigger an inflammatory response. Chronic inflammation can affect the brain and contribute to mental health problems. Research suggests that inflammation in the gut can lead to the release of cytokines, which can cross the blood-brain barrier and influence brain activity.
The overgrowth of bacteria in the small intestine can impair the absorption of essential nutrients, including B vitamins, magnesium, and zinc. These nutrients are essential for brain function, and their deficiency can lead to mental health issues, including anxiety, depression, and cognitive decline.
SIBO can lead to poor gut motility, which means the digestive system does not function properly. This can cause bloating and discomfort, which increases stress and affects mood. The stress from digestive discomfort can trigger or exacerbate mental health conditions, forming a vicious cycle.
SIBO often leads to intestinal permeability (commonly referred to as "leaky gut"). When the lining of the small intestine becomes damaged, toxins and bacteria can leak into the bloodstream, triggering inflammation and potentially affecting the brain, leading to mental health disturbances.
People with SIBO often experience a combination of physical and mental symptoms. Understanding the connection between gut and brain dysfunction can help identify when SIBO is playing a role in mental health.
If you suspect that SIBO is affecting your gut-brain connection and contributing to mental health symptoms, here are several steps you can take to restore balance:
Probiotics may help replenish good bacteria in the gut, but they should be used cautiously in individuals with SIBO. Some types of probiotics may exacerbate symptoms. Always consult a healthcare provider before introducing probiotics into your regimen.

SIBO is a condition that affects far more than just your gut—it can also significantly impact your mental well-being. By understanding how SIBO disrupts the gut-brain connection, you can take proactive steps toward managing the condition and improving both your digestive and mental health. Whether through medical treatments, dietary changes, or stress management, there are effective strategies to regain control and restore balance.
If you suspect that SIBO is affecting your mental health, consulting a gastroenterologist and seeking comprehensive treatment is crucial for achieving relief and improving overall quality of life.
Yes, SIBO can disrupt the gut-brain connection, leading to lower levels of serotonin and increased inflammation, which can result in anxiety, depression, and mood disorders.
If you experience chronic digestive discomfort along with symptoms such as brain fog, fatigue, anxiety, or depression, it may indicate that SIBO is contributing to mental health problems.
Yes, addressing the underlying SIBO through diet, antibiotics, and gut-healing protocols can reduce symptoms of anxiety and depression by restoring balance in the gut-brain connection.
The Low FODMAP Diet is commonly recommended for managing SIBO, as it reduces fermentable carbohydrates that exacerbate digestive symptoms. A balanced, anti-inflammatory diet can also support mental health.
Herbal treatments, such as oregano oil, garlic extract, and berberine, can help manage SIBO. Additionally, probiotics, gut-healing supplements, and stress-reducing practices like meditation can improve mental health outcomes.
Yes, brain fog is a common symptom of SIBO. The gut-brain axis, when disrupted, can lead to cognitive impairments, such as memory difficulties, lack of focus, and confusion.