
Hematemesis (vomiting blood) is a serious symptom that indicates gastrointestinal (GI) bleeding, which may arise from several sources such as peptic ulcers, esophageal varices, and gastritis. One significant risk factor for GI bleeding and hematemesis is alcohol consumption.
Excessive alcohol intake can lead to a range of GI issues that contribute to vomiting blood. Alcohol causes irritation and inflammation in the stomach lining and can also increase the risk of esophageal varices, which are enlarged veins in the esophagus. When these varices rupture, they can lead to massive bleeding, which may manifest as hematemesis.
In this blog, we’ll explore how alcohol consumption is linked to gastrointestinal bleeding and hematemesis, the specific risks associated with heavy drinking, and strategies to prevent alcohol-related GI bleeding.
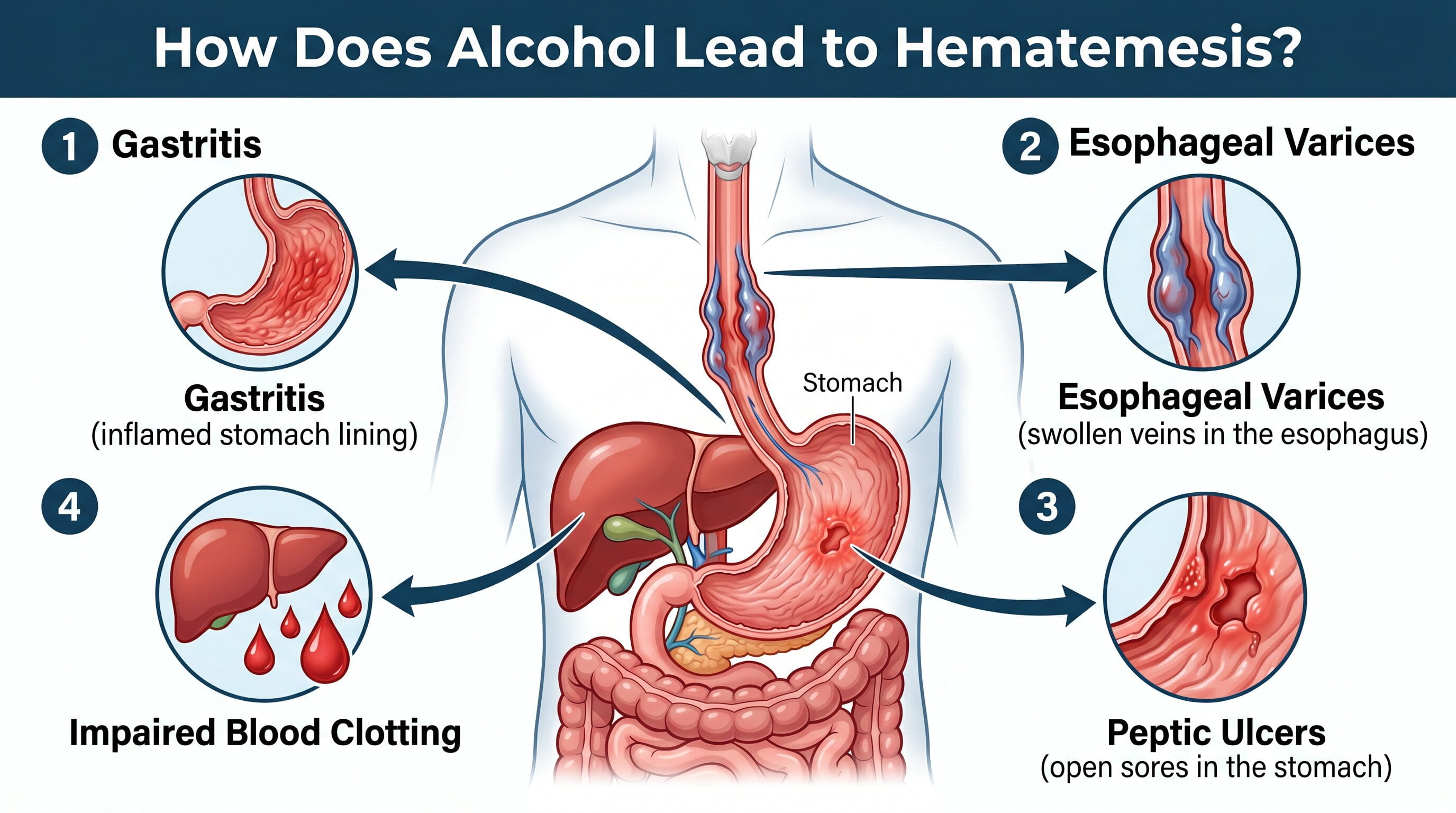
Alcohol affects the gastrointestinal system in multiple ways, all of which can increase the risk of bleeding and vomiting blood. Here’s how alcohol contributes to hematemesis:
Gastritis is the inflammation of the stomach lining, and it is one of the most common alcohol-related causes of hematemesis. Alcohol irritates the mucosal lining of the stomach, increasing acid production and making the stomach more susceptible to damage. Chronic alcohol use can lead to erosive gastritis, where the lining of the stomach becomes worn down, leading to ulcers, bleeding, and the potential for vomiting blood.
Esophageal varices are swollen veins in the lower esophagus that are prone to rupture. They often occur as a result of portal hypertension, a condition commonly associated with liver cirrhosis, which is linked to chronic alcohol use. When these varices rupture, they can cause massive bleeding, resulting in vomiting blood (hematemesis).
Excessive alcohol intake can irritate the stomach lining and increase the production of stomach acid, which may lead to the development of peptic ulcers. These ulcers can bleed if they erode into blood vessels, resulting in hematemesis. Alcohol can also interfere with the healing of existing ulcers, prolonging bleeding.
Heavy alcohol consumption can also impair blood clotting by affecting the liver’s ability to produce clotting factors. This makes it more difficult for the body to stop bleeding, exacerbating the effects of gastrointestinal bleeding and increasing the likelihood of hematemesis.
Alcohol-related hematemesis often comes with additional symptoms due to the underlying conditions causing the bleeding. Common signs include:
The connection between alcohol consumption and hematemesis underscores the serious risks associated with excessive drinking. These risks include:
When a patient presents with hematemesis and a history of alcohol use, doctors will perform several tests to determine the underlying cause of bleeding:
Endoscopy is the gold standard for diagnosing the cause of hematemesis. It allows doctors to directly visualize the esophagus, stomach, and duodenum to identify bleeding sources such as ulcers, varices, or tumors. For alcohol-related bleeding, endoscopy can confirm the presence of esophageal varices or gastritis.
Blood tests are essential for assessing the extent of blood loss and evaluating liver function. A complete blood count (CBC) will check for anemia due to blood loss, and liver function tests will help assess the damage caused by alcohol consumption.
In some cases, imaging studies like a CT scan may be used to assess the liver and esophagus, particularly if a patient has liver disease or cirrhosis. These studies help detect complications like varices or liver damage.
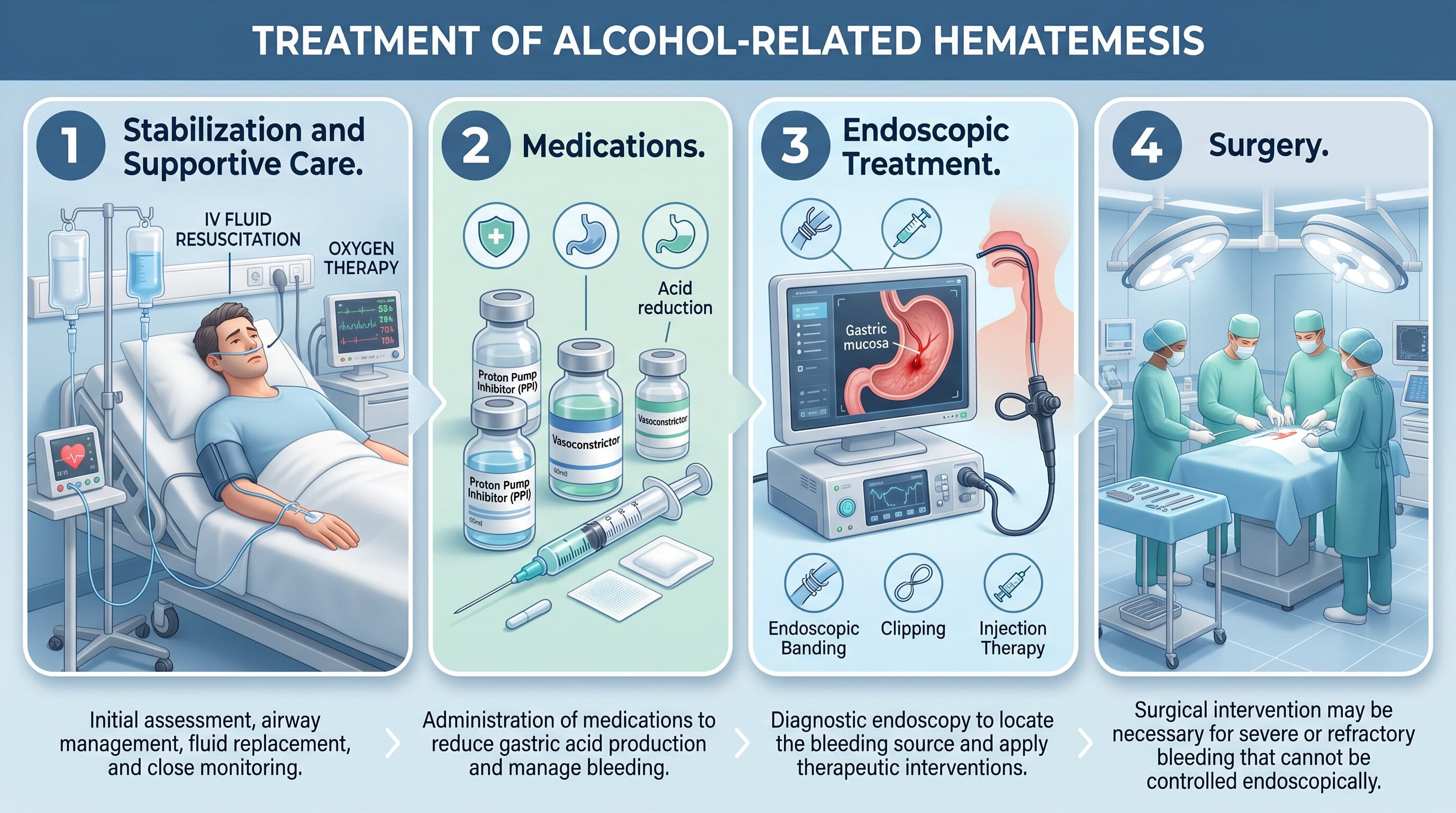
Treatment for alcohol-related hematemesis focuses on both stopping the bleeding and addressing the underlying cause. Here’s how doctors typically approach the treatment:
In emergency cases, patients will be stabilized with IV fluids and possibly blood transfusions to replace lost blood. Monitoring vital signs, including heart rate and blood pressure, is essential to prevent shock.
In severe cases where bleeding cannot be controlled with endoscopic treatment, surgery may be required. This is particularly true for patients with liver disease or large, recurrent ulcers.
The best way to prevent alcohol-related hematemesis is to reduce or eliminate alcohol consumption. Here are some additional tips to protect your GI health:
Alcohol consumption is a significant risk factor for hematemesis, particularly when it leads to gastritis, peptic ulcers, or esophageal varices. While hematemesis caused by alcohol-related conditions is treatable, prevention through responsible drinking and early intervention is key to maintaining GI health and avoiding life-threatening complications.
Yes, excessive alcohol consumption can lead to conditions like gastritis, ulcers, and esophageal varices, all of which can cause bleeding and lead to vomiting blood (hematemesis).
Chronic alcohol use can lead to liver disease and portal hypertension, which can cause esophageal varices to develop. These varices are fragile and can rupture, leading to severe bleeding and hematemesis.
Treatments include IV fluids, blood transfusions, proton pump inhibitors (PPIs) to reduce stomach acid, endoscopic procedures to stop bleeding, and medications like beta-blockers to treat esophageal varices.
Yes, the best prevention is limiting alcohol consumption, quitting smoking, and seeking medical treatment for liver disease. Regular check-ups with a doctor can help monitor the health of your GI tract and liver.
Alcohol-related hematemesis can be life-threatening if not treated promptly. It’s important to seek immediate medical attention if you vomit blood, especially if it’s accompanied by other symptoms like dizziness or abdominal pain.