
When it comes to gastrointestinal (GI) bleeding, two important terms that often arise are hematemesis (vomiting blood) and melena (black, tarry stools). While both are related to internal bleeding in the GI tract, they differ in appearance, origin, and diagnosis.
Hematemesis is a direct sign of upper GI bleeding, while melena typically indicates that the blood has been in the digestive tract long enough to undergo digestion, usually originating from the upper GI tract as well. Understanding these terms is essential in recognizing the severity of the condition and when medical intervention is needed.
In this blog, we will dive into the distinctions between hematemesis and melena, explore their causes, and discuss how they are diagnosed and treated.
Hematemesis refers to vomiting blood, which can occur for various reasons, all pointing to some level of gastrointestinal distress. The blood in vomit may appear as:
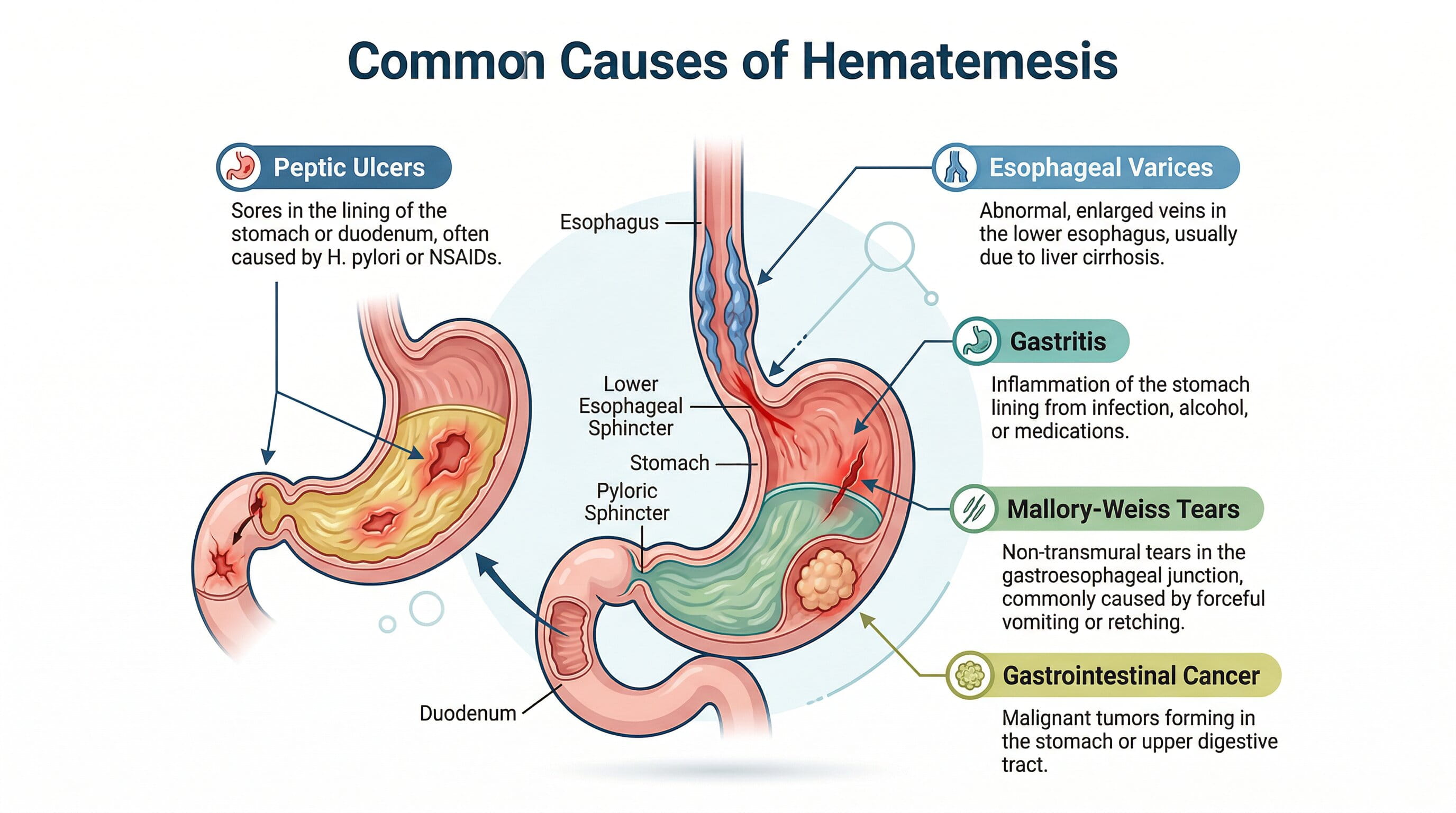
Hematemesis is most commonly caused by:
Melena, on the other hand, refers to black, tarry stools caused by the digestion of blood that has been in the gastrointestinal tract for some time. As blood moves through the stomach and intestines, it is broken down by digestive enzymes and stomach acids, turning it dark. The black color and tarry consistency of the stool are key indicators that blood has been present in the GI tract for a longer period.
Melena usually suggests bleeding from the upper GI tract, which includes the esophagus, stomach, or duodenum. While hematemesis is the immediate result of bleeding, melena signifies that blood has moved further down the digestive system.
Common causes of melena include:
While both hematemesis and melena are signs of gastrointestinal bleeding, they present differently and provide valuable clues to their sources.
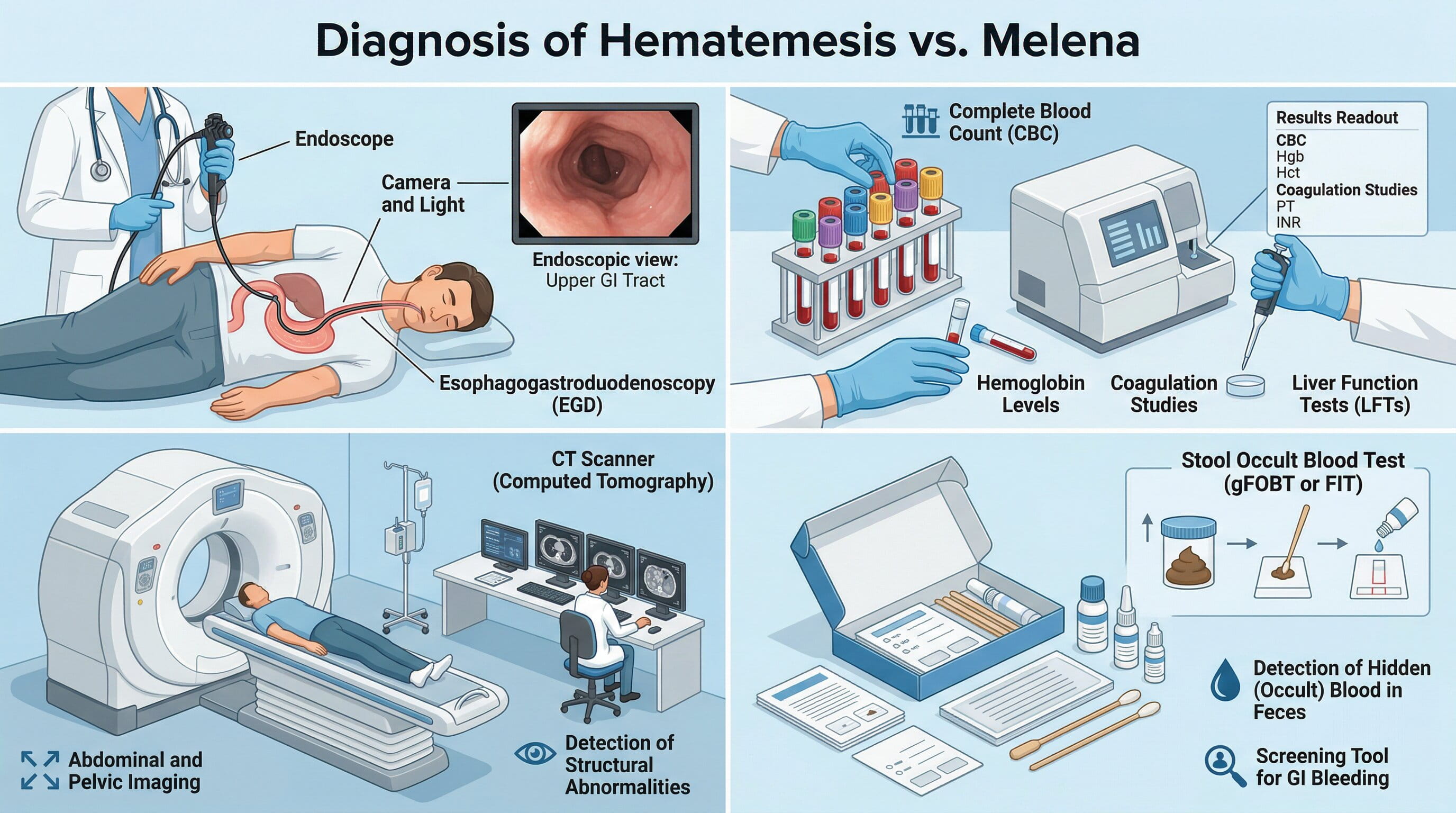
Both hematemesis and melena require immediate medical evaluation to determine the source of bleeding and appropriate treatment. Here’s how doctors diagnose each condition:
The most common diagnostic tool for both conditions is an upper GI endoscopy, where a flexible tube with a camera is inserted through the mouth to examine the esophagus, stomach, and duodenum. This procedure helps identify the source of bleeding, whether it’s from an ulcer, varices, or a tear.
Blood tests are important in assessing the severity of blood loss. Complete blood count (CBC) can help determine if the patient is anemic due to blood loss, while liver function tests can check for conditions like cirrhosis, which could cause esophageal varices.
In some cases, additional imaging like a CT scan may be used to identify sources of bleeding, particularly if endoscopy is inconclusive or if a tumor is suspected.
For melena, doctors may perform a fecal occult blood test (FOBT) to check for hidden blood in the stool, even before the blood is visible.
Treatment for both hematemesis and melena depends on the underlying cause of the bleeding. However, the general approach includes stabilizing the patient, addressing the source of bleeding, and preventing recurrence.
In cases where bleeding cannot be controlled with medications or endoscopy, surgery may be required, such as for gastric cancer or severe ulcers.
Both hematemesis and melena should be taken seriously and prompt medical attention is necessary if:
While hematemesis and melena both indicate upper GI bleeding, they differ in how the blood is expelled from the body and how long it has been in the digestive tract. Understanding the differences between these two symptoms, recognizing the underlying causes, and seeking immediate medical care can help prevent serious complications. If you experience either of these symptoms, it is critical to get evaluated by a healthcare provider for proper diagnosis and treatment.
Hematemesis refers to vomiting blood, while melena refers to black, tarry stools caused by digested blood. Both are signs of upper gastrointestinal bleeding but differ in appearance and the stage of digestion.
Yes, melena can occur without hematemesis if blood from the upper GI tract is slowly digested and passed through the intestines. This can happen in conditions like ulcers, gastritis, or cancer.
Treatment involves stabilizing the patient, stopping the bleeding (often via endoscopy), and addressing the underlying cause, such as ulcers or varices. Medications like PPIs or beta-blockers may also be used.
Melena often indicates chronic or slow bleeding, but it doesn’t always signify a life-threatening situation. It can be caused by conditions like peptic ulcers or gastritis, which are treatable.
Doctors use endoscopy, blood tests, and imaging studies like CT scans to identify the source of bleeding in cases of hematemesis and melena.